Bel Marra Health’s weekly health news roundup consists of stories on fibromyalgia, multiple sclerosis, sebaceous cysts, and skin rashes. This week, we share with you natural remedies for fibromyalgia skin disorders, a new treatment for depression using LSD, new study on multiple sclerosis being triggered by brain cell death, and the similarities and differences between multiple sclerosis and fibromyalgia.
 Fibromyalgia skin disorders, home remedies for painful skin rashes and skin itching
Fibromyalgia skin disorders, home remedies for painful skin rashes and skin itching
Many people who suffer from fibromyalgia also experience skin disorders, including problems that cause skin rashes and skin itching. While the root cause of fibromyalgia and associated skin issues continues to be studied, there is relief for sufferers in the way of home remedies.
Advertisement
Fibromyalgia is best described as chronic widespread pain. It impacts about 10 million Americans. Since there has never been a definitive biological explanation for the condition, only theories, some have suggested it is more of a psychological disability than a physical one.
There is a lot of examination into the mystery behind fibromyalgia. One of the latest discoveries, published in the journal Pain Medicine, concludes that there is a physical link to fibromyalgia, and it’s through the skin.
Researchers at Albany Medical College uncovered “peripheral neurovascular pathology” in the skin of women with fibromyalgia that could explain the deep tissue pain and skin tenderness associated with the condition.
One of the researchers described finding excessive sensory nerve fibers around blood vessel structures in the palms of hands, as opposed to the brain. A few years ago, scientists discovered nervous system function among blood vessels in the skin. Continue reading…
 New LSD study opens depression treatment path using opioid system for major depression relief
New LSD study opens depression treatment path using opioid system for major depression relief
New LSD study opens depression treatment path using opioid system for major depression relief. Researchers at Imperial College London recently published images of the brain under the influence of lysergic acid diethylamide (LSD) from their research set to explore the effects of psychedelic drugs.
For the study, the researches selected participants with a prior history of LSD use. The subjects received either 75 micrograms of LSD or a drug-free placebo. After the injection, the participants underwent a series of tests. The researchers used functional MRI scans to look at areas with increased blood flow. They found a slight increase of the blood flow to the visual cortex, which led to hallucinations experienced while on LSD.
The researchers also used an alternative imaging technique known as magnetoencephalography in order to track the electrical activity in the brain. The researchers noted the changes in the brain’s synchrony, which is the neurons’ ability to fire together. They found that the areas of the brain that usually fire all their neurons in sync stopped doing so under the influence of LSD, while other areas that usually do not fire their neurons together started doing so.
After the brain scans, the researchers gave the participants questionnaires to document their experiences while on LSD. The researchers found ego-dissolution, a feeling of connection with the world around them rather than as a separate entity, is associated with a reduction of brain synchrony. Continue reading…
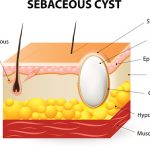 Sebaceous cyst, noncancerous small lump behind the ear, beneath the skin
Sebaceous cyst, noncancerous small lump behind the ear, beneath the skin
A sebaceous cyst is a noncancerous lump behind the ear, which develops underneath the skin, and while it can be unsightly and sometimes uncomfortable, it’s generally not harmful.
Usually a lump behind the ear, a sebaceous cyst can also show up on the head, back, face, breast, and other parts of the body. They tend to appear most often on the face, neck, and trunk. They are small or large. Some people who get a sebaceous cyst find that they have no problems with it and require no treatment, but in some situations the cyst can rub up against clothing or other body parts, can rupture or get infected, causing discomfort. In certain cases, a person may decide to have a cyst surgically removed. Continue reading…
 Multiple sclerosis may be triggered by brain cell death causing an autoimmune response against myelin
Multiple sclerosis may be triggered by brain cell death causing an autoimmune response against myelin
Multiple sclerosis (MS) may be triggered by the death of myelin-producing brain cells (oligodendrocytes), which causes an autoimmune response against myelin. The findings come from researchers at the University of Chicago and Northwestern Medicine who developed novel mouse models to conduct their study. The researchers found that the death of oligodendrocytes initiates an autoimmune response against myelin, triggering multiple sclerosis-like symptoms in mice.
On the other hand, the researchers found that the reaction can be prevented using the specially developed nanoparticles even after the loss of brain cells. These nanoparticles are now being developed in clinical trials with prospects for future treatments in humans.
Co-senior author Brian Popko said, “Although this was a study in mice, we’ve shown for the first time one possible mechanism that can trigger MS — the death of the cells responsible for generating myelin can lead to the activation of an autoimmune response against. Protecting these cells in susceptible individuals might help delay or prevent MS.”
Advertisement
In their genetically engineered mouse model, the researchers targeted the myelin-producing cells. After oligodendrocytes were killed, the mice experienced multiple sclerosis-like symptoms that impaired their walking ability. But after this event, the nervous system started regenerating the oligodendrocytes once again, which allowed the mice to resume walking. After six months, however, the mice experienced difficulty walking again, the researchers noted. Continue reading…
 Fibromyalgia vs. multiple sclerosis (MS), comparing symptoms, diagnosis, and treatment
Fibromyalgia vs. multiple sclerosis (MS), comparing symptoms, diagnosis, and treatment
While fibromyalgia and multiple sclerosis (MS) do share the symptom of pain, fibromyalgia is a musculoskeletal condition and multiple sclerosis is a neurological condition. There is still much unknown about the exact cause of fibromyalgia, but it is believed that the condition increases one’s sensitivity to pain. The cause of multiple sclerosis is the destruction of myelin, the protective coating surrounding nerves. Multiple sclerosis is an autoimmune disease, meaning, the body mistakenly attacks itself. Over time, due to myelin destruction, the nerves can no longer function properly, which results in a slew of symptoms.
Both disorders are debilitating and can negatively affect a person’s quality of life. Furthermore, both conditions can result in chronic pain. And yet, despite their shared similarities, they are two unique conditions with different symptoms, diagnostic processes, and treatment methods. Continue reading…
