 Approximately 42 million American adults suffer from some sort of sleep breathing disorder, with obstructive sleep apnea being the most common type affecting Americans today. It occurs as a result of collapsed soft tissue that blocks the passage of air needed to breath properly. Because this issue is so prevalent, we at Bel Marra have decided to bring you a sleep apnea update. You will also learn how frequent urination and an increased heart failure risk are related to the condition.
Approximately 42 million American adults suffer from some sort of sleep breathing disorder, with obstructive sleep apnea being the most common type affecting Americans today. It occurs as a result of collapsed soft tissue that blocks the passage of air needed to breath properly. Because this issue is so prevalent, we at Bel Marra have decided to bring you a sleep apnea update. You will also learn how frequent urination and an increased heart failure risk are related to the condition.
Diabetics with obstructive sleep apnea at increased risk of blindness: Study
Type 2 diabetes is a serious metabolic condition with a multitude of negative side effects. One of the leading causes of type 2 diabetes is obesity, and many obese individuals also suffer from obstructive sleep apnea (OSA), a potentially dangerous disorder that causes breathing to repeatedly stop and start during sleep.
Advertisement
A new study into patients who have both conditions has found an increased risk for the development of another condition called diabetic retinopathy, which leads to blindness.
“Despite improvements in glucose, blood pressure, and lipid levels, diabetic retinopathy remains very common. Meanwhile, OSA has been shown to be very common in patients with type 2 diabetes, which is not surprising considering that excess weight contributes to the development of both of these conditions,” said corresponding author Dr. Abd Tahrani of the University of Birmingham’s Institute of Metabolism and Systems Research. Continue reading…
 Your smartphone can analyze your sleep-wake cycle
Your smartphone can analyze your sleep-wake cycle
Smartphone device may assess your sleep-wake cycle and help your monitor your obstructive sleep apnea (OSA). Researchers from Ben-Gurion University of the Negev (BGU) developed a system of monitoring sleep-wake cycle among patients by simply using the patient’s smartphone.
Dr. Yaniv Zigel, head of BGU’s Biomedical Signal-Processing Research Lab (BSP) and Professor Ariel Tarasiuk, head of the Sleep-Wake Disorders Unit at Soroka University Medical Center in Beer-Sheva, explained, “We’ve developed technology that could help diagnose OSA and sleep disorders in a convenient way. The audio analysis application can record speech signals from awake subjects. Now, we will be able to get a fast, OSA severity estimation without an overnight sleep study.” Continue reading…
 Frequent night awakenings and urination may be due to obstructive sleep apnea, not enlarged prostate
Frequent night awakenings and urination may be due to obstructive sleep apnea, not enlarged prostate
Frequent night awakenings and urination may be caused by obstructive sleep apnea, rather than enlarged prostate. The study compared men aged 55 and 75 years old with an enlarged prostate diagnosis who reported nighttime urination (nocturia) at least once a night. The control group did not have prostate enlargement or nocturia.
The study found that over half of the patients with an enlarged prostate may have a sleep disorder, which could actually be the reason for nocturia, rather than the enlarged prostate.
Researcher Dr. Howard Tandeter said, “If nocturia severity in BPE [benign prostate enlargement] patients is actually a pre-existing sleep disorder, this can now be treated and help improve patients’ quality of life. Even among those patients with well-defined medical reasons for nocturia, sleep disorders may still be found as the source of most awakenings from sleep. Therefore, the diagnosis of a sleep disorder should be seriously considered whenever a patient reports frequent awakenings from sleep to urinate, since the problem is treatable.” Continue reading…
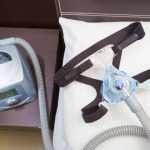 Obstructive sleep apnea patients with CPAP intolerance may benefit from hypoglossal nerve stimulation (HGNS)
Obstructive sleep apnea patients with CPAP intolerance may benefit from hypoglossal nerve stimulation (HGNS)
Advertisement
Obstructive sleep apnea patients with CPAP intolerance may benefit from hypoglossal nerve stimulation (HGNS). Continuous positive airway pressure (CPAP) device is commonly used to treat sleep apnea. A facial mask worn throughout the night, it produced continuous airflow to make sure the person doesn’t stop breathing. Some individuals, however, may be intolerant to CPAP device – which means they cannot effectively treat sleep apnea and thus are at a higher risk for associated health complications.
The solution to a CPAP intolerance may be a device implanted in the chest known as hypoglossal nerve stimulation (HGNS). Continue reading…
 Obstructive sleep apnea may increase heart failure and death in women
Obstructive sleep apnea may increase heart failure and death in women
Obstructive sleep apnea may increase heart failure and mortality in women. Risk factors for both sleep apnea and heart failure do differ between men and women, and it has been unclear whether the effects of sleep apnea on cardiovascular health were the same for both sexes. To establish any differences, researchers evaluated the links among sleep apnea, cardiac bio-markers that provide early evidence of heart disease, and occurrence of adverse heart outcomes in 1,625 individuals who were free of heart disease when first studied and followed for an average of almost 14 years.
The findings suggest, there are gender-based differences between obstructive sleep apnea and cardiovascular disease. In women specifically, sleep apnea was associated with higher blood levels of troponin, a marker that provides information on early evidence of heart injury. Continue reading…
