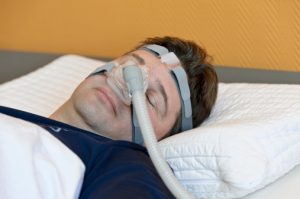
 Sleep apnea, sleep disordered breathing (SBD), has been linked to an increased stroke risk. Sleep disordered breathing is a condition characterized by a group of disorders, which involve abnormal respiratory patterns or insufficient ventilation during sleep.
Sleep apnea, sleep disordered breathing (SBD), has been linked to an increased stroke risk. Sleep disordered breathing is a condition characterized by a group of disorders, which involve abnormal respiratory patterns or insufficient ventilation during sleep.
Apnea is a condition where breathing is halted for roughly 10 seconds or more and the person becomes wakes up to catch their breath.
Advertisement
Hypopnea is where breathing becomes shallow and is associated with oxygen desaturation or arousal.
In both cases sleep patterns are disrupted, leaving the individual feeling tired in the morning and can put excessive strain on the nervous system and other organs.
Types of sleep disordered breathing
 There are three main types of sleep disordered breathing: obstructive sleep apnea, central sleep apnea and mixed sleep apnea.
There are three main types of sleep disordered breathing: obstructive sleep apnea, central sleep apnea and mixed sleep apnea.
Obstructive sleep apnea occurs when the upper airway closes either partially or fully, but breathing attempts to continue. Causes of obstructive sleep apnea include lack of muscle tone during sleep, excessive tissue in the upper airways and the structure of the upper airway and jaw.
Central sleep apnea is when the upper airway is open, but respiratory efforts cease due to a decrease in respiratory drive. Central sleep apnea is a nervous system disorder and can also be caused by stroke, brain tumor, viral brain infection or chronic respiratory disease.
Unlike obstructive sleep apnea, snoring is not a characteristic of central sleep apnea, so it can go undiagnosed for years.
Lastly, mixed sleep apnea is when signs of both obstructive and central sleep apnea are present.
The growing evidence linking sleep disordered breathing and stroke
 The link between sleep disordered breathing and stroke only came to light in the 1990s. Sleep apnea is commonly found in individuals after experiencing a stroke. Between 1996 and 2010 over 20 different studies showed an association between stroke and SDB. A 2010 analysis of 29 studies revealed that the type of stroke did not affect SDB prevalence, but individuals with multiple strokes had higher rates of SDB. Furthermore, males were more affected by SDB than women.
The link between sleep disordered breathing and stroke only came to light in the 1990s. Sleep apnea is commonly found in individuals after experiencing a stroke. Between 1996 and 2010 over 20 different studies showed an association between stroke and SDB. A 2010 analysis of 29 studies revealed that the type of stroke did not affect SDB prevalence, but individuals with multiple strokes had higher rates of SDB. Furthermore, males were more affected by SDB than women.
More recent findings uncovered that obstructive sleep apnea is seen within 50 percent of stroke sufferers. Furthermore, having obstructive sleep apnea increases the risk of stroke, dependent on other factors, including smoking, obesity and diabetes.
The latest findings also support that the use of a continuous positive airway pressure (CPAP) machine can help reduce the risk of recurrent stroke in those who have sleep apnea and a history of stroke.
Sleep apnea can cause brain damage
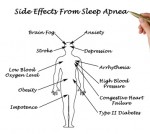 A study conducted by researchers at UCLA found that sleep apnea can cause brain damage. When oxygen intake is reduced to the brain it contributes to damage, and this is what researchers found to be true in patients with sleep apnea. Principal investigator, Rajesh Kumar, said, “We found that the blood–brain barrier becomes more permeable in obstructive sleep apnea, a breakdown that could contribute to brain injury, as well as potentially enhancing or accelerating the damage.”
A study conducted by researchers at UCLA found that sleep apnea can cause brain damage. When oxygen intake is reduced to the brain it contributes to damage, and this is what researchers found to be true in patients with sleep apnea. Principal investigator, Rajesh Kumar, said, “We found that the blood–brain barrier becomes more permeable in obstructive sleep apnea, a breakdown that could contribute to brain injury, as well as potentially enhancing or accelerating the damage.”
The researchers used magnetic resonance to observe the damage done to the blood-brain barrier in those with sleep apnea. The blood-brain barrier protects the brain from infection, chemicals and other threats. They found those who were recently diagnosed with sleep apnea, but were not receiving treatment, were at greater risk of a compromised blood-brain barrier when compared to healthy individuals.
Kumar concluded, “This suggests that besides improving breathing in obstructive sleep apnea patients, we need to repair or improve blood-brain barrier function, perhaps by using treatments already available for other conditions.”
Daytime and nighttime symptoms of SDB-related brain damage
Key symptoms and factors of SDB include being obese and reporting excessive daytime sleepiness – but sometimes these two factors are not present. In particular, in those with an underlying cardiovascular problem, symptoms may reveal themselves quite differently.
Nighttime symptoms of sleep disordered breathing are:
- Difficulties falling asleep
- Snoring
- Irregular or periodic respiration
- Apnea – stoppage of breathing
- Disrupted sleep with frequent awakenings
- Sudden awakenings or choking
- Shortness of breath
- Palpitations or panic attacks
- Orthopnea
- Increased sweating
Daytime symptoms of sleep disordered breathing are:
 Headache
Headache- Fatigue
- Excessive daytime sleepiness
- Difficulties with memory or concentrating
- Irritability
- Depression
- Breathing irregularities
Lifestyle and home remedies to prevent sleep apnea
If you want to lower your risk of stroke and other complications associated with sleep apnea, it’s important to prevent sleep apnea. Here are some lifestyle and home remedies to prevent sleep apnea.
- Lose excess weight.
- Exercise regularly.
- Avoid alcohol and certain medications, such as sleeping pills.
- Sleep on your side or abdomen as opposed to your back.
- Keep nasal passages open at night.
- Stop smoking.
Related Reading:
Depression in adults reduced with CPAP therapy for sleep apnea
In adults with obstructive sleep apnea, treatment with a continuous positive airway pressure therapy (CPAP) therapy can improve depressive symptoms. Depression is commonly seen in individuals with obstructive sleep apnea, so by treating the sleep apnea they can reduce their risk of depression. Continue reading…
Advertisement
Diagnosing sleep apnea in women may be helped by new symptom
Bedwetting has been found to be a helpful symptom when trying to diagnose post-menopausal women with obstructive sleep apnea, according to new findings. The lead author of the study suggests that nearly two percent of post-menopausal women suffer from sleep apnea – a condition where a person can stop breathing while they are asleep. Continue reading…
Sources:
http://www.resmed.com/us/en/healthcare-professional/diagnosis-and-treatment/sleep-disordered-breathing
http://www.resmed.com/us/en/healthcare-professional/diagnosis-and-treatment/sleep-disordered-breathing/types-of-sleep-disordered-breathing
http://www.acc.org/latest-in-cardiology/articles/2015/06/25/08/24/evolving-relationship-between-sleep-disordered-breathing-and-stroke
//www.belmarrahealth.com/obstructive-sleep-apnea-can-cause-brain-damage-study
http://www.mayoclinic.org/diseases-conditions/sleep-apnea/basics/lifestyle-home-remedies
