March is the National Colorectal Cancer Awareness Month, and as we are reaching the end of this month, why not review some of the relevant and pressing topics, such as what can increase your colon cancer risk, inflammatory bowel disease (IBD), and chronic inflammation. Colorectal cancer is now the fourth most common form of cancer and it is most frequently seen in individuals over the age of 50. Regular screening, especially for those at higher risk, can help reduce incidences of colorectal cancer.
Here are Bel Marra Health’s news stories regarding colorectal cancer, from information regarding stool tests to obesity as a risk factor and even colorectal cancer screening guidelines – everything you need to know about colorectal cancer.
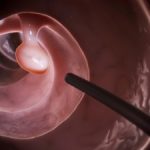 Obesity increases risk of colon cancer, link uncovered
Obesity increases risk of colon cancer, link uncovered
Advertisement
Although it is well known that obesity increases the risk of colon cancer, the exact link has never been quite fully understood. New research has now looked further into the link between obesity and colon cancer and has uncovered the biological connection, which could lead to better treatment and preventative options in the future.
The study was conducted on mice, where researchers found that a high-calorie diet turned off a key hormone in the intestine, which deactivates a tumor suppressor pathway. Researchers noted that genetically replacing the hormone turned it back on, which prevent cancer development.
The findings of the study reveal the benefits of a pill known as linaclotide (Linzess), which is structurally related to the lost hormone as a means of preventing colon cancer in obese patients.
Study’s senior author Scott Waldman said, “Our study suggests that colorectal cancer can be prevented in obese individuals with use of hormone replacement therapy — much as other diseases associated with hormone deficiency, such as loss of insulin in diabetes, can be treated.” Continue reading…
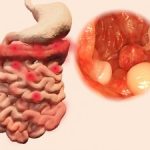 IBD-related colorectal cancer risk raised by chronic inflammation, immunosuppressive therapy
IBD-related colorectal cancer risk raised by chronic inflammation, immunosuppressive therapy
Inflammatory bowel disease-related colorectal cancer risk is raised by chronic inflammation and immunosuppressive therapy. The review was conducted by Dr. Laurent Beaugerie from Hôpital Saint-Antoine in Paris and Dr. Steven H. Itzkowitz from Icahn School of Medicine at Mount Sinai.
In the news release, the researchers said, “Among the chronic inflammatory diseases that often require the prolonged use of immunosuppressants, [inflammatory bowel disease] is an intriguing model because immunosuppressants may reduce the incidence of inflammation-related cancers through their anti-inflammatory effects or promote immunosuppression-related cancers.”
Individuals with inflammatory bowel disease (IBD) have 1.5 times higher risk of developing colon cancer, compared to the general population.
A previous meta-analysis study has found that an improved control of inflammation, along with frequent colonoscopies and the use of chemopreventive 5-aminosalicylates (5-ASAs), promoted a decrease in the higher risk for colon cancer in IBD patients. However, other studies have made conflicting conclusions with regards to the preventative effect of 5-ASAs.
Roughly 15 percent of colon cancers are diagnosed within the first seven years of IBD diagnosis. It is also well known that chronic inflammation plays a role in colitis-associated cancer.
Data on Crohn’s disease suggests that patients with Crohn’s have a 20 to 30 percent higher risk of bowel adenocarcinoma in ileal lesions after eight years of diagnosis, compared to the general public. The only preventative measure in Crohn’s patients is to remove the ileal lesions. Continue reading…
 Changes in colorectal cancer screening guidelines suggested for aging seniors
Changes in colorectal cancer screening guidelines suggested for aging seniors
Changes have recently been suggested to colorectal cancer screening guidelines for aging seniors. Colorectal cancer is estimated to claim the lives of up to 50,000 Americans this year alone. An effective way to reduce fatalities linked to colon cancer is through preventative screening. New research argues that scheduling colonoscopy screenings for seniors every five years is not justifiable for many patients, even those who have a family history of colon cancer.
The researchers followed 144,768 men and women, between the ages of 55 and 74, over the course of 13 years. The goal was to determine colon cancer risk in those with a family history of colon cancer by at least a first degree relative.
Those with an average risk are advised to undergo a colonoscopy every 10 years after the age of 50. Those who have a first degree relative who had colon cancer and are younger than 60, or who have two relatives with colon cancer at any age, are recommended to undergo a colonoscopy every five years, beginning at the age of 40 or 10 years prior to the age their youngest relative was diagnosed with colon cancer. Screening is usually recommended to stop between 75 to 85 years of age, but it has been unclear if this is useful or not. Continue reading…
 1 in 7 colon cancer patients diagnosed prior to screening age
1 in 7 colon cancer patients diagnosed prior to screening age
New research has found that one in seven colon cancer cases are being diagnosed prior to the screening age – with typical screening age above 50 years. The new findings suggest that those under the age of 50 were more likely to have advanced stages of the disease, which researchers suggest occurs because their cancer is only diagnosed once symptoms begin.
Advertisement
Study author, Samantha Hendren, said, “Colorectal cancer has traditionally been thought of as a disease of the elderly. This study is really a wake-up call to the medical community that a relatively large number of colorectal cancers are occurring in people under 50. To put this in context, breast cancer screening often begins at age 40, and less than 5 percent of invasive breast cancers occur in women under that age. Our study found that about 15 percent of colorectal cancers are diagnosed before the screening age of 50.” Continue reading…
 Stool test effective for detecting colon cancer
Stool test effective for detecting colon cancer
A stool test has been found to be an effective means in detecting colon cancer, according to the latest findings. The test looks for blood in stool and can be conducted on an annual basis. Researchers believe that stool testing is not only effective, but is a safer, more cost-effective mode of testing compared to colonoscopy.
When examining stool, doctors look for microscopic amounts of blood, which are shed from colon tumors. There is a concern that stool testing may become less effective over time compared to screening, as only larger tumors shed blood, and if the tumor is removed it may make stool testing less effective.
In order to achieve their findings, researchers tracked annual fecal blood tests performed on nearly 325,000 patients over the course of four years. Continue reading…
