 Giant cell arteritis in elderly is linked to the herpes virus causing chicken pox and shingles. Giant cell arteritis is a condition in which the blood vessels in the temples and scalp become inflamed, which can lead to sudden blindness or stroke.
Giant cell arteritis in elderly is linked to the herpes virus causing chicken pox and shingles. Giant cell arteritis is a condition in which the blood vessels in the temples and scalp become inflamed, which can lead to sudden blindness or stroke.
Study author Don Gilden said, “Our analysis, which is the largest to-date, provides compelling evidence that the virus also reactivates in people over 60 in another way, triggering giant cell arteritis.”
Advertisement
Giant cell arteritis is the most common blood vessel inflammation in seniors, affecting nearly 29 out of 100,000 people.
The researchers examined 13 temporal artery biopsies of people who have died with no previous symptoms of giant cell arteritis and another 84 biopsies of people who had the condition to find evidence of chicken pox and shingles virus.
Varicella zoster virus – herpes virus – was found in 74 percent of biopsies from the giant cell arteritis group and eight percent in the group without the condition.
In a corresponding editorial, Peter Kennedy wrote, “If the association in this landmark study can be replicated in other studies, clinical trials should focus on treating people with giant cell arteritis with a combination of the current steroid drugs used for the condition, plus antiviral treatment for the virus.”
Giant cell arteritis symptoms, causes, and risk factors
The exact cause of giant cell arteritis is unknown, but researchers believe it is linked to the body’s autoimmune response. Furthermore, excessive dosages of antibiotics and certain severe infections have been tied to contributing to giant cell arteritis. Prevention is difficult because the exact cause is unknown. But once arteritis is detected, treatment can aid in reducing complications associated with the condition.
Symptoms of giant cell arteritis include:
- Double vision
- Sudden, permanent loss of vision
- Throbbing headache in the temples
- Fatigue
- Weakness
- Loss of appetite
- Jaw pain, especially when chewing
- Fever
- Unintentional weight loss
- Shoulder and hip pain or stiffness
- Tenderness of scalp and temple area
Giant cell arteritis is commonly seen in individuals over 50, so age is a large risk factor. Women are also more likely to develop giant cell arteritis, compared to males. Whites of Northern European or Scandinavian descent are at higher risk, compared to other races.
Lastly, having a condition known as polymyalgia rheumatica or having a family history of giant cell arteritis also increases the risk of developing the condition.
Giant cell arteritis prevention and home remedies
As mentioned, prevention for giant cell arteritis isn’t possible as researchers and doctors are still unaware of its cause. There are things you can do though to better manage the condition. The following tips can help cope with side effects from treatment medications and aid with symptoms.
- Eat a healthy diet to protect bones, treat high blood pressure, and manage diabetes.
- Exercise regularly.
- Check in with your doctor regularly in order to prevent complications.
- Talk to your doctor about taking a daily dose of aspirin to reduce the risk of stroke and blindness.
Giant cell arteritis treatment and diagnosis
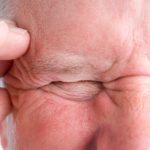 To diagnose giant cell arteritis, doctors rely heavily on the manifestation of symptoms along with a physical examination. During the examination, the doctor may notice that the temple region is sensitive to touch and has a faint pulse. This can prompt them to conclude that the condition is giant cell arteritis.
To diagnose giant cell arteritis, doctors rely heavily on the manifestation of symptoms along with a physical examination. During the examination, the doctor may notice that the temple region is sensitive to touch and has a faint pulse. This can prompt them to conclude that the condition is giant cell arteritis.
Accompanying tests that can be performed to further assist in diagnosis include blood work, eye exam, temporal artery biopsy, and cranial ultrasound.
The best form of treatment for giant cell arteritis is the prescription of corticosteroids. A common corticosteroid used in treatment is known as prednisolone, which may first be injected and later prescribed in tablets. Prednisolone may be taken for up to two years in order to eliminate and manage symptoms. Even though symptoms may disappear after a few days of taking the medications, it’s important that you follow through with the treatment as the symptoms may reappear.
Although corticosteroids like prednisolone are effective, they do come with side effects. Some common side effects of prednisolone include:
- Increased appetite and, in turn, weight gain
- Increase in blood pressure
- Mood changes
- Weakened bones
- Stomach ulcers
- Increased risk of infection
Other medications that may be prescribed are low-dose aspirin and immunosuppressants. As mentioned, regular follow-ups should be made with your doctor in order to prevent complications related to giant cell arteritis and to make any necessary changes to your medication. You should never stop taking a medication unless instructed otherwise by your health care provider.
Related Reading:
Heart disease, stroke risk in women higher if artery disease-causing gene present
Heart disease and stroke risk in women is higher if an artery disease-causing gene is present. Heart disease is the primary cause of death within the U.S., and a person dies from a heart disease-related event every minute. To prevent heart attack, it’s important to understand what increases a person’s risk. Continue reading…
Advertisement
Oral bacteria increase hemorrhagic stroke risk
Oral bacteria have been found to increase the risk of hemorrhagic stroke. Within a single hospital, the researchers studied the patients admitted for stroke to uncover an association between oral bacteria and hemorrhagic stroke. In patients who experienced intracerebral hemorrhage (ICH), 26 percent were found to have a specific bacterium in their saliva known as cnm-positive Streptococcus mutans. Continue reading…
Sources:
https://www.aan.com/PressRoom/Home/PressRelease/1342
http://www.healthline.com/health/temporal-arteritis#Diagnosis3
http://www.mayoclinic.org/diseases-conditions/giant-cell-arteritis/basics/risk-factors/con-20023109
http://www.arthritis.org/about-arthritis/types/giant-cell-arteritis/
http://www.mayoclinic.org/diseases-conditions/giant-cell-arteritis/basics/lifestyle-home-remedies/con-20023109
http://www.nhs.uk/Conditions/giant-cell-arteritis/Pages/Diagnosis.aspx
http://www.nhs.uk/Conditions/giant-cell-arteritis/Pages/Treatment.aspx
