May is Celiac Awareness Month, which highlights not only the condition but the significance of a gluten-free diet. Celiac disease is a condition in which the immune system attacks gluten as if it were a threat when it enters the body, causing negative side effects.
There are many other factors that relate to celiac disease aside from gluten, including pneumonia, osteoporosis, dementia, and coronary artery disease. For these reasons, we have compiled a list of our top editorials discussing celiac disease and eating a gluten-free diet.
 Gluten-free diet can relieve brain fog in celiac disease patients
Gluten-free diet can relieve brain fog in celiac disease patients
Advertisement
A gluten-free diet can relieve brain fog in celiac disease patients. Common symptoms of celiac disease include abdominal pain, constipation, diarrhea, and cramping, but another symptom, which is often overlooked, is brain fog.
When a person experiences brain fog, they feel fatigued and tired, they may fumble during conversations, their thoughts may appear slower, and they lack creativity. If severe, a person may even completely mess up things that are very familiar to them, for example, how to get home from a destination.
Because brain fog in celiac disease is not a commonly discussed symptom, it often goes overlooked. And yet, many celiac patients report brain fog being lifted once they go gluten free.
In a study published in the Alimentary Pharmacology and Therapeutics, researchers found cognitive ability to improve once patients began a gluten-free diet. The study was conducted on 11 newly diagnosed celiac patients who were tested for information-processing efficacy, memory, visuospatial ability, motor function, and attention before starting them on a gluten-free diet.
After 12 weeks of being on the diet, the patients were tested again, and once more after one year. Blood testing, intestinal permeability tests, and small bowel biopsies via gastroscopy were also conducted at baseline, week 12, and week 52.
Improvements were seen in all four cognitive tests with adherence to a gluten-free diet. Corresponding author Gregory W. Yelland said, “This study, while small in numbers, does provide objective evidence for the cognitive impairments associated with untreated coeliac disease. We would like to think that clinicians would use this to inform their patients of the cognitive risks of remaining untreated and of the benefits of adhering to a strict gluten-free diet, for not only their physical [health,] but their mental health also.”
The authors wrote, “If these findings are confirmed in a larger study, they may have important health and safety implications. When viewed together, the present results indicate that short-term memory, movement, and processing speed are impaired in untreated [celiac disease,] and that they improve during adherence to a [gluten-free diet].” Continue reading…
 Pneumonia risk higher in celiac disease patients not vaccinated against the infection: Study
Pneumonia risk higher in celiac disease patients not vaccinated against the infection: Study
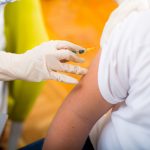
Pneumonia risk is higher among celiac disease patients who are not vaccinated against the infection. The study compared 9,803 celiac patients with 101,755 controls, and the rate of pneumonia was found to be similar. But the researchers did find a 28 percent increased risk in celiac patients who were unvaccinated, compared to the controls.
The increased risk was seen in patients younger than 65, was highest around the time their celiac disease had been diagnosed, and was maintained for over five years after diagnosis. Only 26.6 percent of the patients were vaccinated after being diagnosed with celiac disease. The authors wrote, “As only a minority of patients with celiac disease are being vaccinated, there is a missed opportunity to intervene to protect these patients from pneumonia.”
Celiac disease patients may be at a greater risk of pneumonia due to a diminished spleen function, which can affect the pneumonia-causing bacteria. Continue reading…
 Celiac disease increases osteoporosis and bone fracture risk
Celiac disease increases osteoporosis and bone fracture risk
Celiac disease increases the risk of osteoporosis and bone fractures. The findings were presented at the EULAR 2011 Annual Congress, where researchers announced that celiac disease patients have a 4.5 times greater risk of developing osteoporosis, compared to healthy individuals of the same age and gender.
The study compared bone mineral density (BMD) loss in two physical locations in the body in 1,030 people. The researchers found that the lumbar spine BMD in celiac disease patients was significantly different in comparison to the control group. The femoral neck bone mineral density, however, was not found to be significantly different than the control group.
Mr. Oldroyd of Lancaster University School of Medicine said, “This is the first study that compares the extent of BMD loss at the lumbar spine and femoral neck in an age- and sex-matched cohort, and demonstrates that the detrimental effects of coeliac disease are most pronounced in the lower back compared to the hip joint. These findings may be due to the fact that the bone in the lumbar spine is spongy, less dense and weaker in comparison to the femoral neck, causing it to be more susceptible to the detrimental effects of coeliac disease. There is greater research required to determine why this effect is seen and whether it can have future implications for treatment.” Continue reading…
 Celiac disease patients may face higher coronary artery disease risk
Celiac disease patients may face higher coronary artery disease risk
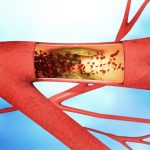
Celiac disease patients may face a higher coronary artery disease risk compared to those without the disease. The risk in celiac patients was found to increase twofold, compared to the general population. The study also revealed a slightly higher risk of stroke in celiac patients as well.
Coinvestigator of the study R.D. Gajulapalli, M.D., said, “People with celiac disease have some persistent low-grade inflammation in the gut that can spill immune mediators into the bloodstream, which can then accelerate the process of atherosclerosis and, in turn, coronary artery disease. Our findings reinforce the idea that chronic inflammation, whether it’s from an infection or a disease, can have an adverse role in coronary artery disease and heart health in general.”
Researchers examined medical records of patients from 13 different hospitals where 24,530 were diagnosed with celiac disease. Patients without celiac disease were the controls. Smoking status and diabetes prevalence were fairly the same across both groups. Celiac patients were slightly more inclined to have higher cholesterol, but less likely to have high blood pressure. Common risk factors for celiac disease include gender, race, diabetes, smoking, high cholesterol, and high blood pressure.
There was a slightly higher prevalence of coronary artery disease among celiac patients. Dr. Gajulapalli added, “This is an important study because it highlights a specific patient population who might be at higher risk for coronary artery disease, even in the absence of traditional cardiovascular risk factors. We were surprised by the strength of the association, especially in younger people. Patients and doctors should be aware of this association.”
“Whether patients with celiac disease will need more intense risk factor modification like in diabetic patients with coronary artery disease will need to be studied,” Dr. Gajulapalli concluded.
Larger studies are required in order to confirm the findings as well as examine how the severity of celiac disease affects the risk of coronary artery disease. Continue reading…
 Dementia risk in celiac disease patients does not increase before or after their diagnosis
Dementia risk in celiac disease patients does not increase before or after their diagnosis
Dementia risk in celiac disease patients does not increase before or after diagnosis. Director of the Celiac Disease Center Peter Green said, “Patients coming to our center have long described ‘brain fog,’ and it appears that gluten can cause cognitive effects in some individuals with and without celiac disease. However, we didn’t know if these effects have long-term consequences in the form of increased risk of dementia.”
The study analyzed 8,846 individuals over the age of 50 with celiac, along with matched controls without celiac disease, in order to determine the incidence rate of dementia. After an average 8.4-year follow-up, dementia was diagnosed in 4.3 percent of celiac patients and 4.4 percent of the matched controls.
Advertisement
Lead author Benjamin Lebwohl said, “Celiac disease did not increase the risk of Alzheimer’s in this population-based study. We did not find evidence of increased dementia risk prior to the diagnosis of celiac disease, either.”
Celiac disease was not found to increase the risk of Alzheimer’s dementia, but there was a slight increase in vascular dementia. Dr. Lebwohl added, “We know that patients with celiac disease have a modestly increased rate of cardiovascular disease, and that patients who experience neurologic symptoms have abnormalities on MRIs that mimic vascular disease.”
Dr. Green concluded, “People who promote an anti-grain or anti-gluten agenda sometimes cite our work in celiac disease, drawing far-ranging conclusions that extend well beyond evidence-based medicine. We know ‘brain fog’ is a serious symptom commonly reported by our patients, and it’s understandable that people have been worried about a possible connection to dementia. Fortunately, our work with Dr. Ludvigsson provides concrete evidence that this particular worry can be laid to rest.” Continue reading…
