 Bruised ribs can be a result of broken (fractured) ribs, but there are other causes too. One thing is for sure, no matter how you developed the condition, it is often painful and can make laying down—or even breathing and moving in certain positions—difficult.
Bruised ribs can be a result of broken (fractured) ribs, but there are other causes too. One thing is for sure, no matter how you developed the condition, it is often painful and can make laying down—or even breathing and moving in certain positions—difficult.
An injured or fractured rib is often a result of some type of trauma, whether it is a fall or a direct blow to the chest. Unlike other bones in the body, you cannot put a broken rib in a cast, so taking the necessary steps at home to nurse your ribs back to health is highly important.
What causes bruised ribs?
Advertisement
As mentioned, there are several causes for bruised ribs, including an injury to the chest such as one resulting from physical sports, vehicular accident, or repeated coughing either from pneumonia, whooping cough, or bronchitis.
Knowing the cause of your bruised ribs can help you better treat them at home and can also help your doctor put you on a treatment plan.
Understanding bruised ribs symptoms
Symptoms that can be experienced with bruised ribs include tenderness or pain when the area is touched, extreme pain when breathing, shortness of breath, increased pain when moving, sharp constant pain, visible bruising, difficulty sleeping or laying on the affected area, and inflammation that results in chest pains.
Diagnosing bruised ribs
Once your doctor takes a complete history of the events leading up to the injury as well as a physical exam, they may find it necessary to do some tests to see the extent of the damage and rule out any additional injuries that have also occurred. The following are such tests:
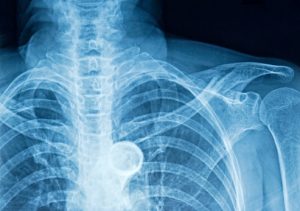
Anteroposterior (AP) and lateral chest X-ray: Great for looking at the structure of the rib cage and routinely assisting in diagnosis and ruling out fractures. Several underlying injuries can also be ruled out with this test, such as hemothorax, pneumothorax, lung contusion, atelectasis, pneumonia, and vascular injuries.
Chest CT: A more sensitive imaging test compared to an X-ray, a computerized tomography (CT) scan may be done as an additional test if the diagnosis is inconclusive. It is optimal for determining the number of ribs involved, the coverage of the injury, and can help diagnosis injuries beyond the ribs themselves.
Angiography: The position of the first and second ribs are in close proximity to vital blood vessels and may cause a vascular injury. This test can assess for any blood vessel injury.
Urinalysis: May aid in finding blood in the urine due to kidney injury.
Arterial blood gasses: Can help assess if the lungs have been badly bruised, affecting their oxygen transferring ability.
Complete blood count (CBC): A routine test for almost all trauma patients, obtaining a CBC can help determine blood loss as well as assess the status of various blood components.
Natural remedies to treat bruised ribs and reduce healing time
Here are a few natural remedies to not only treat bruised ribs but also help reduce healing time.
Check your ribs: First, distinguish between a bruised or broken rib. Rub your hand over the area, and if it feels tender, then it is most likely bruised, but if there are gashes or marks, it may be broken. Consult your doctor to verify whether or not your rib is bruised or broken.
Ice the area: Icing the area can help reduce swelling and pain. Ideally, it’s best to ice the area for up to 72 hours. If pain still persists, switch to warm compresses.
Rest: Having a bruised rib can make breathing and moving quite difficult, so take this time to rest as much as possible to avoid increasing the damage.
Manage your breathing: As mentioned, breathing can be difficult with a bruised rib, so you may have to manage your breathing. Try to breathe as deeply as possible as much as you can. Even if it is quite painful, at least try to get one deep breath in at least once every 60 minutes. If you cannot take a deep breathing once an hour, see a doctor.
Stay mobile in-between the rest periods: Walking around between periods of rest can help promote breathing and clear mucus.
Advertisement
Carry out breathing exercises: Take 10 slow deep breaths every hour, allowing your lungs to inflate fully.
When to see a doctor for bruised ribs
If pain is persistent over the course of a few weeks, you should check in with your doctor to see what is going on. Other signs that can prompt you to see your doctor include an increasing shortness of breath, increasing chest pain, pain in the stomach or shoulder, coughing up blood, coughing up green or yellow mucus, and a fever.
These symptoms could indicate a chest infection, which requires medical intervention.
