 Ischemic colitis is when blood flow to the colon becomes reduced; therefore, atherosclerosis contribute to ischemic colitis by narrowing the arteries. This lack of blood flow to the colon limits the supply of oxygen for the cells in the digestive system.
Ischemic colitis is when blood flow to the colon becomes reduced; therefore, atherosclerosis contribute to ischemic colitis by narrowing the arteries. This lack of blood flow to the colon limits the supply of oxygen for the cells in the digestive system.
Ischemic colitis can be misdiagnosed as other digestive issues and can heal on its own. Ischemic colitis can turn into an infection, so medication is required to prevent this. If damage is done to the colon, surgery may be required.
Ischemic colitis causes
Advertisement
It isn’t always clear as to why blood flow becomes reduced to the colon, but there are factors that can increase the risk of it, such as:
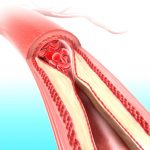 Atherosclerosis
Atherosclerosis- Hypoglycemia
- Blood clot
- Bowel obstruction caused by a hernia
- Surgery that involves blood vessels
- Medical conditions affecting the blood, such as lupus or sickle cell anemia
- Cocaine or methamphetamine use
- Colon cancer
In rare cases, certain medications can contribute to ischemic colitis as well. Those medications include:
- Some heart and migraine medications
- Hormone medications
- Antibiotics
- Pseudoephedrine
- Certain medications for irritable bowel syndrome
- Chemotherapy
Ischemic colitis symptoms
Symptoms of ischemic colitis are:
 Pain, tenderness or cramping in the abdomen
Pain, tenderness or cramping in the abdomen- Bright-red or maroon colored stool
- Feeling of urgency to release bowels
- Diarrhea
- Nausea
When symptoms are on the right side of the abdomen there is a higher risk of complications. The arteries on the right side also supply blood to the small intestine, which can also be blocked. Pain in this area is generally much worse.Blocked blood flow to the small intestine can become deadly. Surgery is required in order to remove the blockage.
Risk Factors and Complications of Ischemic Colitis
Risk factors for ischemic colitis include being older in age, having clotting abnormalities, high cholesterol, reduced blood flow due to heart failure or low blood pressure, undergoing a previous abdominal surgery, heavy exercise such as marathons, and undergoing surgery that involves the aorta (large artery).
If not treated, ischemic colitis can result in complications including death of the tissue (gangrene), perforation of the intestines, bowel inflammation, or bowel obstruction causing it to be difficult to pass bowel movements.
How to Diagnose Ischemic Colitis
Your doctor will utilize several different tests to properly diagnose ischemic colitis. These different tests include an ultrasound or abdominal CT scan, stool analysis, CT or MRI angiography which provides detailed images of blood flow, and a colonoscopy to provide detailed images of the colon.
Ischemic colitis treatment
The severity of the ischemic colitis decides which treatment will used. Symptoms can subside within days, but your doctor may still prescribe medications as a precaution to prevent infection.
Treatments for ischemic colitis include:
- Antibiotics
- IV fluids to prevent dehydration
- Treatment for underlying medical condition
- Avoiding medications that may constrict blood vessels
If the ischemic colitis is severe, surgery may be required in order to:
- Remove dead tissue
- Repair a hole in your colon
- Bypass blockage in an intestinal artery
- Remove part of the colon that has narrowed due to scarring, which is creating the blockage
Advertisement
Surgery is more likely in those with heart disease or low blood pressure.
Ischemic colitis prevention
It is difficult to prevent ischemic colitis as there are many factors that can contribute to its onset. Some prevention tips include:
- Exercising regularly
- Eating a healthy diet
- Treating heart conditions
- Controlling cholesterol and blood pressure
- Not smoking
By taking the right steps to prevent ischemic colitis, you can not only reduce your risk of the condition, but you are protecting yourself from its harmful complications and living a healthier life.
