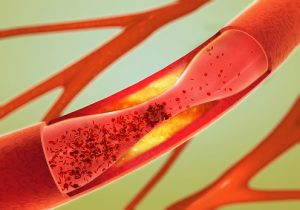
 Rheumatoid arthritis increases the risk of deep vein thrombosis (blood clots in legs) and blood clots in lungs, according to research. The findings revealed that individuals with rheumatoid arthritis – an inflammatory type of arthritis – have triple the risk of developing deep vein thrombosis and double the risk of pulmonary thromboembolism (blood clotting in the lungs), compared to individuals without rheumatoid arthritis.
Rheumatoid arthritis increases the risk of deep vein thrombosis (blood clots in legs) and blood clots in lungs, according to research. The findings revealed that individuals with rheumatoid arthritis – an inflammatory type of arthritis – have triple the risk of developing deep vein thrombosis and double the risk of pulmonary thromboembolism (blood clotting in the lungs), compared to individuals without rheumatoid arthritis.
Dr. Tore Kvien, editor-in-chief of the journal Annals of the Rheumatic Diseases and head of rheumatology at Diakonhjemmet Hospital in Oslo, Norway, said, “I would call this a moderate increased risk.”
Advertisement
“This study is consistent with what our study and other published papers found,” added Dr. Seoyoung Kim, assistant professor of medicine at Brigham and Women’s Hospital and Harvard Medical School in Boston. Dr. Kim’s team also found a similar association in their study.
For the study, researchers used a national database to select 30,000 rheumatoid arthritis patients whom they monitored for the development of blood clots for two years. The data was compared to 117,000 individuals without rheumatoid arthritis.
After adjusting for other risk factors that could lead to blood clots, rheumatoid arthritis patients still had a higher risk of blood clots compared to patients without the condition. Furthermore, patients under the age of 50 were at highest risk.
Although the researchers are unaware of the mechanisms that could link rheumatoid arthritis to blood clots, they suspect that inflammation plays a role.
The researchers suggest that rheumatoid arthritis patients who require surgery, cancer treatment, or hospitalization should be put on a clot-prevention program and follow a healthy lifestyle to further reduce their risk of blood clots.
Rheumatoid arthritis patients at increased risk for blood clots: Previous study
A previous study looked at over 45,000 residents of Sweden with rheumatoid arthritis and found that they had a higher risk of venous thromboembolism. They also found that the risk remained stable over the course of 10 years. The background information of the article stated, “Recent reports suggest that rheumatoid arthritis (RA) may be a risk factor for venous thromboembolism (VTE), particularly in conjunction with hospitalization. Using hospitalization data to identify RA and VTE may identify patients when they are at elevated risk for other reasons, obscuring the incompletely understood underlying association between RA and VTE and leading to inappropriate institution or timing of interventions.”
The authors wrote, “The results of this study suggest that patients with RA are at increased risk of VTE (both deep vein thrombosis and pulmonary embolism) and that the risk of VTE increases shortly after RA diagnosis and remains similarly elevated during the first decade. Hospitalization is a strong risk factor for VTE in the general population and in patients with RA, but the short-term (less than one year after hospital discharge) rates for VTE are similar in both groups. VTE rates varied with age, less so with sex, calendar period of RA diagnosis, and rheumatoid factor status, but the relative risks of VTE were largely similar across these patient subgroups.”
Blood clot treatment and preventive tips
Advertisement
Blood clots can be removed through surgical procedures depending on the underlying cause, but surgery is often reserved for a life- or limb-threatening situation and when anticoagulation medications don’t work. After a blood clot surgery, once again depending on the cause, your doctor will schedule follow-ups, especially if blood thinners are prescribed to monitor dosing.
Prevention tips of blood clots include:
- Managing blood pressure, cholesterol, diabetes, smoking cessation, and managing other risk factors associated with heart disease as they increase the risk of blood clots.
- If you underwent a surgery, it’s important that you begin walking as soon as possible in order to prevent a blood clot.
- Travelers, especially on long flights or car rides, should stretch and move around as much as possible.
- Monitor your hormone therapy as that can increase the risk of clots as well.
By preventing a blood clot you can reduce your risk of blood clot-related complications.
