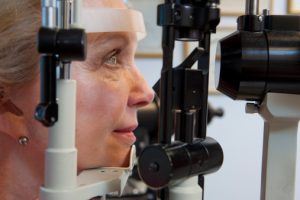
 Glaucoma fall risk in the elderly can be detected early and reduced by measuring gait abnormalities – movement patterns of limbs – according to new findings. Researchers from Washington State University developed a way to analyze a person’s gait with sensors, which could reduce the risk of falls in elderly people with glaucoma.
Glaucoma fall risk in the elderly can be detected early and reduced by measuring gait abnormalities – movement patterns of limbs – according to new findings. Researchers from Washington State University developed a way to analyze a person’s gait with sensors, which could reduce the risk of falls in elderly people with glaucoma.
Researchers from Washington State are working with a team at the University of California, Los Angeles to begin clinical trials to test the sensors.
Advertisement
Graduate student Yuchao Ma said, “Glaucoma is usually diagnosed late but earlier detection of gait disturbances could make a difference.”
Previous research found that glaucoma patients have a greater fall risk as vision deterioration worsens. Glaucoma sufferers tend to walk slower, bump into more objects and have unequal step placement. Unfortunately, many patients are not diagnosed in the early stages when the disease is more easily treatable.
The sensors, which the researchers developed, are worn on shoes to measure, filter and analyze gait information. This allows researchers to examine specific features of movement, such as step length, equity between feet and evenness of step. In clinical trials movements of glaucoma patients are compared to control groups.
Researchers hope the technology will allow for earlier diagnosis of glaucoma. UCLA researchers are now in the process of recruiting participants in different stages of glaucoma for their next set of clinical trials.
Falls due to poor vision
 It’s of no surprise that poor vision can contribute to a higher risk of falls. Poor vision reduces stability and depth perception, and contrast sensitivity increases the risk of falls even more. Numerous research studies point to the notion that poor vision in the elderly can increase their risk of falls, leading to injury and a lower quality of life.
It’s of no surprise that poor vision can contribute to a higher risk of falls. Poor vision reduces stability and depth perception, and contrast sensitivity increases the risk of falls even more. Numerous research studies point to the notion that poor vision in the elderly can increase their risk of falls, leading to injury and a lower quality of life.
The College of Optometrists suggests that one in three seniors over the age of 65 will experience a fall each year, and less than three percent of those questioned about their parent’s falls reported an association with deteriorating vision.
Dr. Susan Blakeney from the college does not believe that failing vision needs to be an inevitable part of aging, she said, “We are concerned that public awareness of the link between poor vision and falls is so low. Suffering a fall can have an extremely debilitating effect on the quality of an older person’s life and the lives of those around them. Being aware of changes in vision is particularly important for those older people at higher risk of falling or who have fallen before.”
Many people who were asked about their parents in a research project known as Opinion Matters were not aware their parents could receive sight tests within their home, or that many sight tests for those over the age of 60 are actually free. The researchers of the study want to ensure this demographic is able to reduce their risk of falls through regular eye examinations. Jane Ashcroft, Chief Executive of Anchor, said, “We are keen to lend our support to any campaign which encourages greater understanding about what causes falls and how to prevent them.”
Dr. Blakeney offered some advice to reduce the risk of falls: “If you have recently had a big change to your spectacle prescription, ask your optometrist whether they can give you a compromise prescription to make it easier for you to get used to it. You should only wear your new spectacles at home until you are used to them. If your optometrist has told you that you should wear spectacles for distance (television, walking about etc), you should keep them on when you are walking outside the home as this could make you less likely to fall.”
“Some people are more likely to fall if they walk about wearing bifocals or varifocals, even if they are used to them. So, if you take part in regular outdoor activities it may be best to have a pair of distance spectacles to wear when walking about outdoors or when you are in unfamiliar places. If your distance vision is good without your spectacles it may be best to take your bifocals or varifocals off for walking about. Your optometrist will be able to advise you about this,” she concluded.
Risk of falls due to glaucoma detected using virtual reality
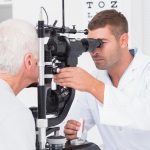 Additional technology was used to detect fall risk in glaucoma patients with the help of virtual reality. The research team from the University of California San Diego studied 42 patients with glaucoma and 38 healthy subjects. First the subject’s balance was recorded without stimulation, then with the use of a black screen and goggles they were presented with stimulated movement.
Additional technology was used to detect fall risk in glaucoma patients with the help of virtual reality. The research team from the University of California San Diego studied 42 patients with glaucoma and 38 healthy subjects. First the subject’s balance was recorded without stimulation, then with the use of a black screen and goggles they were presented with stimulated movement.
During the stimulated movements researchers saw improved balance in glaucoma patients by 30 to 40 percent, compared to the healthy subjects. Researchers also found, “the degree to which balance was lost was strongly linked to a history of falls, which validated the study’s methods and metrics.”
Senior author, Felipe A. Medeiros, M.D., said, “Measures from traditional static visual field tests do not mimic the visual conditions that occur day-to-day. With further refinement of this method, we hope that the approach could one day be used to identify patients at high risk of falling so that preventative measures can be employed at an earlier stage.”
Researchers propose that the loss of balance in glaucoma patients is linked with the loss of retinal ganglion cells, which also contribute to the disease.
The findings were published in Opthalmology.
Prevent glaucoma to reduce fall risk
Advertisement
Falls can negatively impact a senior’s life. Recovery time of injury due to fall takes much longer, they are robbed of the ability to perform daily tasks and it can increase their risk or worsen pre-existing illnesses. For these reasons, it’s important to reduce your risk of falls and the best way to do that is by preventing glaucoma.
 Here are some tips to help you prevent glaucoma, maintain healthy vision and ultimately reduce your risk of falls.
Here are some tips to help you prevent glaucoma, maintain healthy vision and ultimately reduce your risk of falls.
- Get checked – early detection is key and should start as early as 40, over the age of 65 eyes should be checked every six to 12 months.
- Exercise is not only beneficial for overall health, but it can reduce your risk of glaucoma as well.
- Always wear protective eyewear, whether it’s sunglasses, swimming goggles, or goggles, at work to prevent debris from entering your eyes.
Tips for people with low vision to prevent falls
Any changes in vision can increase your risk of falls, so whether you have glaucoma or any other eye condition, here are some tips to reduce your risk of falls.
- Keep rooms well lit.
- Use task lighting when completing daily chores.
- Use nightlights in bedrooms and hallways.
- Put bright colored tape along stairs.
- Paint doorways and light switches a contrasting color to make them easier to see.
- Use light or dark cutting boards depending on the color of food you’re cutting. For example, a white cutting board can be useful for cutting dark food items and vice versa.
- Place plates and food items on contrasting colored placemats.
- Used a pill organizer with raised lettering.
- Keep rooms tidy and ensure objects are placed off to the side and not in the middle of the room.
- Place the television in a spot where daylight and lamplight don’t reflect off of it.
