World Malaria Day is on April 25, and this year’s theme is ending malaria for good. This year, though, a new threat has emerged known as Zika virus, which is another mosquito-transmitted illness. In light of the rise of this virus, it’s important that we educate you on both malaria and Zika, and how either illness can affect conditions like metabolic syndrome and lupus. It’s important to note that individuals with certain health conditions may not benefit from antimalarial medications.
Here are Bel Marra Health’s stories on malaria, malaria vaccines, Zika virus, and other associated conditions.
 Zika virus vs malaria, differences in symptoms, treatment, and prevention
Zika virus vs malaria, differences in symptoms, treatment, and prevention
Advertisement
Zika virus and malaria are both mosquito-borne illnesses, and since the rise of Zika first in Brazil and now overseas, many are questioning the similarities and differences between malaria and Zika virus.
Zika is becoming a growing problem, as it’s not only affecting the Brazil population, but sending worldwide researchers and scientists into frenzy to better understand the virus and develop proper treatments and potentially a cure.
Malaria, on the other hand, has been residing in Africa for decades, and there are effective treatment methods available to address the illness.
Although both Zika virus and malaria are transmitted through mosquitoes, the two illnesses still have their respective differences, which is important to understand. Here is a breakdown of the similarities and differences when it comes to Zika virus and malaria. Continue reading…
 Metabolic syndrome in lupus affecting women prevented by antimalarial drug
Metabolic syndrome in lupus affecting women prevented by antimalarial drug
Metabolic syndrome in lupus affecting women can be prevented by antimalarial drug. A recent study uncovered that an antimalarial drug could be effective in preventing metabolic syndrome in women with lupus. Metabolic syndrome is classified by the National Heart, Lung and Blood Institute as, “a group of risk factors that raises your risk for heart disease and other health problems, such as diabetes and stroke.”
The study, led by Luciana F. Muniz, evaluated the frequency of metabolic syndrome and disease in relation to 103 premenopausal female lupus patients along with 35 healthy premenopausal control women.
Metabolic syndrome was higher among the women with lupus in comparison to the healthy women. The researchers also found that the use of chloroquine – an antimalarial drug – had protective effects against metabolic syndrome in lupus patients. Continue reading…
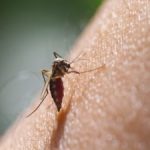 Cure for malaria in testing phase
Cure for malaria in testing phase
A drug currently being tested shows promise as a cure for malaria. Researchers from UT Southwestern Medical Center and researchers in Australia are working together on this potential cure.
Malaria is spread by mosquitoes. It causes fevers, chills, flu-like symptoms, and – in severe cases – death. The mosquitoes spread a parasite that attacks red blood cells. It can also be transmitted through a compromised blood transfusion, though this is very rare. According to the Centers for Disease Control and Prevention, malaria killed about 500,000 people in 2013. Most of these deaths were children in Africa.
The CDC noted about 1,500 cases of malaria are reported in the U.S. every year. Patients are usually visitors or travelers from sub-Saharan Africa and Asia. The drug being tested DSM265 works by killing off the drug-resistant malaria parasites. The targeted parasite is Plasmodium, and so far the drug has been showing promise in preclinical trials.
A need for a new drug to combat malaria is high, as more cases of treatment-resistant malaria are reported.
“The problem is we’re starting to see more drug resistance, and this is what’s taken out every anti-malarial drug we’ve had,” said Dr. Margaret Phillips, professor of pharmacology at UT Southwestern. Continue reading…
 European Medicines Agency approves malaria vaccine
European Medicines Agency approves malaria vaccine
A week ago (July 17, 2015) Bel Marra Health reported about a drug currently being developed by researchers from UT Southwestern Medical Center and researchers in Australia, showing promise as a cure for malaria.
On the heels of that report comes a possible malaria vaccine.
The Committee for Medicinal Products for Human Use (CHMP), a division of the European Medicines Agency (EMA), worked closely with other experts from the World Health Organization (WHO) and regulatory authorities from relevant countries before adopting a positive scientific opinion for Mosquirix, a vaccine for Plasmodium falciparum and hepatitis B.
The recently developed vaccine is intended for the active immunization of children aged six weeks to 17 months against malaria in areas where malaria is regularly found, and also for immunization against hepatitis B.
The malaria vaccine Mosquirix was submitted to EMA to assess its quality, safety, and efficacy, as well as its benefit-risk balance for markets outside of the European Union. However, in its assessment, the CHMP applied the same rigorous standards used for vaccines to be marketed within the EU. In spite of decades of research into malaria vaccinations, Mosquirix is the first malaria vaccine to be assessed by a regulatory agency. Continue reading…
 Crime-scene compound targets malaria parasite
Crime-scene compound targets malaria parasite
In the case of malarial research, ‘crime does pay.’ If everything goes according to the plan for researchers at Washington University School of Medicine in St. Louis, the compound used at crime scenes to find trace amounts of blood may one day be used to kill the malaria parasite.
The new study falls perfectly in sync with WHO guidelines, which suggest that artemisinin — the most commonly used antimalarial drug — only be used in combination with other treatments because the parasite is becoming resistant to it.
The compound luminol glows blue when it reacts with hemoglobin in red blood cells. The researchers have shown that they can use this glow to trick malaria-infected red blood cells into building up a volatile chemical stockpile.
Advertisement
To achieve this, the researchers first gave the infected red blood cells an unusual amino acid and then used the blue glow to trigger the chemical. The strategy worked in killing the parasite.
According to senior author Daniel Goldberg, professor of medicine and molecular microbiology, the blue light that luminol emits is enhanced by the antimalarial drug artemisinin. The results show that we can combine these two agents to form an effective treatment against the malarial parasite.
The results of the study are available online in the journal eLife. Continue reading…
