August is Spinal Muscular Atrophy Awareness Month, so we are presenting to you a selection of our articles on spinal muscular atrophy and related topics, like muscular dystrophy, obstructive sleep apnea, scoliosis, and back pain.
Spinal muscular atrophy (SMA) affects the motor nerves in the spinal cord essentially robbing the sufferers of their strength. SMA can negatively impair one’s ability to walk, eat, or even breathe.
Advertisement
SMA is a genetic mutation of the SMN1 gene. In healthy individuals, this gene produces a protein that is critical for normal nerve functioning. An SMA patient cannot produce enough of this protein, meaning, the nerves can’t properly function and eventually die.
 Spinal muscular atrophy cause uncovered by stem cell research
Spinal muscular atrophy cause uncovered by stem cell research
The cause of spinal muscular atrophy, a condition that leads to muscle weakness, has been uncovered by stem cell research. The findings come from researchers at the Advanced Gene and Cell Therapy Lab at Royal Holloway.
The researchers used stem cell techniques to get a better understanding as to why some cells are at a higher risk of degenerating in spinal muscular atrophy than others.
The researchers used Induced Pluripotent Stem Cells (iPSCs), which were reprogrammed and coerced into forming motor neurons that are found in the spine to help control movement and breathing.
During the differentiation stage when the stem cells change into their final shape, two key proteins in motor neurons change in a significant way, which could help explain why these cells are more vulnerable to spinal muscular atrophy degeneration than others. Continue reading…
 Muscular dystrophy treatment with muscle damage repair shows promise
Muscular dystrophy treatment with muscle damage repair shows promise
Muscular dystrophy treatment with muscle damage repair shows promise. Muscular dystrophy is a group of diseases that cause progressive muscle weakness and loss of muscle mass. Abnormal genes interfere with the production of proteins needed to make healthy muscles.
There are different types of muscular dystrophy. In some, symptoms present themselves in childhood, and in others symptoms only emerge in adulthood. Over time, muscular dystrophy can impair a person’s ability to walk. Some people may have difficulties swallowing or breathing.
There is currently no cure for muscular dystrophy, but treatments can help manage the condition and slow down its progression. Continue reading…
 Obstructive sleep apnea common after spinal injury
Obstructive sleep apnea common after spinal injury
Obstructive sleep apnea (OSA) is common after a spinal injury. The study suggests that patients who experienced a spinal injury could benefit from a sleep assessment test to diagnose sleep apnea.
The results of the study showed that 77 percent of spinal cord injury patients have symptomatic sleep-disordered breathing and 92 percent have poor sleep quality. More specifically, there are high rates of obstructive sleep apnea among those with sleep-disordered breathing.
Dr. Abdulghani Sankari, lead author, said, “The majority of spinal cord injury survivors have symptomatic sleep-disordered breathing and poor sleep that may be missed if not carefully assessed. Our findings help in identifying the mechanism of sleep-disordered breathing in spinal cord injury and may provide potential targets for new treatment.”
“Sleep-disordered breathing may contribute to increased cardiovascular mortality in spinal cord injury patients. All spinal cord injury patients should undergo a comprehensive sleep evaluation using full, overnight polysomnography for the accurate diagnosis of sleep apnea,” added Dr. M. Safwan Badr who was also involved in the study.
The researchers studied 26 chronic spinal cord injury patients who all underwent baseline spirometry, filled out a number of questionnaires, and attended polysomnography with flow and pharyngeal pressure measurements. Continue reading…
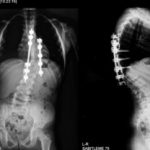 Scoliosis, an abnormal spine curvature in adolescence, may also affect older adults
Scoliosis, an abnormal spine curvature in adolescence, may also affect older adults
Scoliosis in adults is an abnormal spine curvature, also known as degenerative scoliosis.
Degenerative scoliosis is the gradual deterioration of the facet joints, also seen in osteoarthritis of the spine. The main difference between degenerative scoliosis and osteoarthritis of the spine is that pressure from the deteriorating facet joints in degenerative scoliosis causes the spine to curve off to one side.
There are two main categories of adult scoliosis: adult idiopathic scoliosis and adult “de novo” or degenerative scoliosis. In adult idiopathic scoliosis, the patient developed scoliosis as a child or adolescent, but because there is no known cause for scoliosis, it is idiopathic. “De novo” or degenerative scoliosis is the degeneration of the facet joints, where a person can lose height as the spine curves to one side.
Advertisement
Studies on adult scoliosis have shown a prevalence of the condiiton as high as 68 percent among seniors, and the risk factors are directly associated with disability. Continue reading…
 Exercise improves back pain by boosting spine muscles
Exercise improves back pain by boosting spine muscles
Exercise designed to boost coordination of the spine muscles can reduce back pain, according to the latest findings. The program, called motor control exercise, begins with the patient practicing normal use of the spine muscles by conducting regular tasks and activities under guidance of a physical therapist. Exercises gradually become more intense and difficult and can include movements that the patient may use during work or recreational activities.
The researchers analyzed data from 29 clinical trials involving over 2,400 people who suffered from lower back pain between the ages of 22 and 55. Effectiveness of motor control exercise was evaluated in comparison with other form of exercise as well as absence of any exercise. Continue reading…
