 Arteries take blood from the heart and transport it throughout the body. Veins, on the other hand, return this blood back to the heart where it can be recycled. In most cases, we talk more about arteries as they can become clogged, which can increase the risk for a cardiovascular-related event or stroke. Veins can get clogged, too, and if they aren’t treated early on, it can cause a slew of health consequences as well.
Arteries take blood from the heart and transport it throughout the body. Veins, on the other hand, return this blood back to the heart where it can be recycled. In most cases, we talk more about arteries as they can become clogged, which can increase the risk for a cardiovascular-related event or stroke. Veins can get clogged, too, and if they aren’t treated early on, it can cause a slew of health consequences as well.
One condition that can affect veins is known as phlebitis, which occurs when a superficial vein system becomes swollen and inflamed. There is also spontaneous phlebitis, where swelling and inflammation occurs suddenly.
Advertisement
Here we will outline more about phlebitis, including the causes, symptoms, and how you can reduce your risk.
What is phlebitis: Causes, symptoms, treatment
Phlebitis refers to inflammation of the vein. When this is caused by blood clots, it’s known as thrombophlebitis. Phlebitis may result from a medical or surgical procedure, injury to the vein, prolonged inactivity, obesity, smoking, having certain medical conditions, hormone replacement therapy, or taking oral contraceptives, pregnancy, or varicose veins.
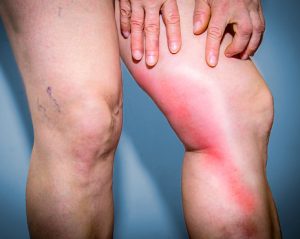
Symptoms of phlebitis include a gradual reddening of the skin, the area may feel warm, hard, or tender to touch, the skin around the vein may be itchy or swollen, and the area may begin to throb or burn. Symptoms can be worse in the morning and some patients experience a low-grade fever.
For some types of phlebitis, symptoms may not be present, which can delay diagnosis and treatment, increasing the risk of complications.
When you begin to experience swelling, pain, and inflammation, and it doesn’t resolve itself after two weeks, you should seek medical attention. If you experience a high fever, lumps in your leg, severe pain or swelling in the leg or arm, and unexplained shortness of breath, seek medical attention as soon as possible. These are signs of a blood clot, which can very quickly become deadly.
Advertisement
In many cases, you can treat phlebitis at home by taking anti-inflammatory medications and applying heat to the affected area—never ice! Your doctor will also recommend you partake in exercises that increase blood circulation like walking, as this prevents blood clots. Your doctor will also recommend you wear compression socks so that blood does not pool in your legs. You will want to avoid long periods of inactivity as this can worsen symptoms and cause complications.
Medical treatment for phlebitis includes blood thinners or antibiotics in cases where it is caused by an infection.
Some ways to lower your risk of phlebitis is to reduce your risk factors which I mentioned, along with staying hydrated, controlling your weight, exercising regularly, and eating an anti-inflammatory diet.
Related: Poor circulation: Common causes, symptoms, and diagnosis tips
