June is National Migraine and Headache Awareness Month, so we have compiled our articles discussing migraines and headaches as well as related factors like irritable bowel syndrome, fibromyalgia, and carpal tunnel syndrome.
The articles below examine issues surrounding migraines and headaches independently and in relation to other health conditions, too.
Advertisement
We hope you enjoy these informative articles and that you gain a greater awareness with regards to migraines and headaches that plague so many Americans.
 Migraines, tension headaches, and irritable bowel syndrome share common genetic links: Study
Migraines, tension headaches, and irritable bowel syndrome share common genetic links: Study
Migraines, tension headaches, and irritable bowel syndrome (IBS) have been found to share a common genetic link. Irritable bowel syndrome is a gastrointestinal disorder that affects nearly 45 million people in the U.S. The exact cause of IBS is still unknown and many patients can go undiagnosed for years. Symptoms of IBS include bloating, diarrhea, constipation, and abdominal pain.
Study author Dr. Derya Uluduz said, “Since headache and irritable bowel syndrome are such common conditions, and causes for both are unknown, discovering a possible link that could shed light on shared genetics of the conditions is encouraging.”
The study involved 107 individuals with episodic migraines, 53 tension-type headaches, 107 people with IBS, and 53 healthy individuals as controls. Migraine and tension headache patients were examined for IBS, and IBS patients were asked about headaches.
The researchers found that migraine patients were twice as likely to have IBS, compared to tension headache patients – 54 migraine patients had IBS, compared to 28 tension headache patients. Thirty-eight IBS patients had migraines and 24 had tension headaches.
Researchers observed the serotonin transporter gene and the serotonin receptor 2A gene. They found that in IBS, migraine, and tension headache patients, there was at least one gene that differed from the genes of the control patients.
Dr. Uludiz added, “Further studies are needed to explore this possible link. Discovering shared genes may lead to more future treatment strategies for these chronic conditions.” Continue reading…
 Fibromyalgia, the risk of migraine and other primary headaches
Fibromyalgia, the risk of migraine and other primary headaches
Fibromyalgia, a condition characterized by widespread chronic pain, has been associated with migraine headaches.
People who have fibromyalgia experience various symptoms, including pain, anxiety, depression, fatigue, mental fog, and morning stiffness. Another common complaint among sufferers is migraines. Research shows that almost all people with fibromyalgia will suffer a migraine at some point; some will experience headaches on a regular basis. Migraine headaches, along with the symptoms of fibromyalgia, can be very difficult to cope with.
This is how fibromyalgia and migraine syndrome have been explained by neurologists:
When inflammation results due to pain, the brain reacts with ionic activity. This can happen to anyone, but for people who have fibromyalgia, the pain is even worse. Migraines that occur in those with fibromyalgia are often much more intense than those without the condition. Also, some people complain that their original fibromyalgia symptoms get worse as the migraine intensifies.
Fibromyalgia and migraine headaches can be debilitating. There is no cure for fibromyalgia, and when it comes to migraines, all you can do is treat the pain once the headache strikes. Special medications and lifestyle changes, such as reducing stress, adjusting diet, exercising, and incorporating alternative therapies like acupuncture, can often relieve the pain associated with the headaches. Continue reading…
 Carpal tunnel syndrome and migraine headaches, study shows association between the two
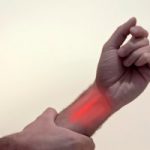
Carpal tunnel syndrome and migraine headaches, study shows association between the two
An association has been found between carpal tunnel syndrome and migraine headaches. A study has found that carpal tunnel sufferers are twice as likely to suffer from migraine headaches as those without the condition. Additionally, the association is also seen in migraine headache sufferers having a higher risk of suffering from carpal tunnel syndrome. The findings work as evidence to support the idea that nerve decompression surgery may be an effective means to treat migraine headaches.
For the study, researchers analyzed data from close to 26,000 Americans who responded to a national health survey. Part of the questions asked whether a person had carpal tunnel syndrome during the past year and whether they had experienced migraine headaches during that time.
Based on definitions, 3.7 percent of respondents had carpal tunnel syndrome and 16.3 percent had migraine headaches. After further analysis, researchers found that patients who suffered from migraine headaches had a higher risk of carpal tunnel syndrome and vice versa. Migraine headaches were found in 34 percent of carpal tunnel syndrome patients, in comparison to 16 percent without carpal tunnel syndrome. Furthermore, the odds of suffering a migraine headache with carpal tunnel syndrome were 2.6 times higher, compared to those without the condition.
Both migraine headaches and carpal tunnel syndrome patients were found to share similar risk factors, including being female, being obese, being diabetic, being of older age, and being a smoker. What is important to note is that Asians had the lowest risk for both conditions and Hispanics had a lower risk of carpal tunnel syndrome.
Previous research has explored the benefits of relieving compressed nerves as a means to alleviate migraine headaches, but the idea is highly controversial. The new findings help support this notion by revealing the association between carpal tunnel syndrome and migraine headaches.
Migraine headaches commonly affect those of younger age, but can really affect anyone. Carpal tunnel syndrome commonly affects those of older age. Because of this, further research will explore if migraine headaches are an early indicator for later-life carpal tunnel syndrome. Continue reading…
 Cluster headache pain and comparison with migraine headaches
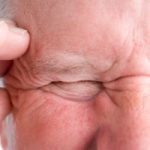
Cluster headache pain and comparison with migraine headaches
Cluster headaches and migraines both cause pain, but they are two different conditions. A cluster headache is a headache that occurs several times in a day, it is short in length and very painful. Cluster headaches may only affect one side of the head, and pain is usually felt around the eyes.
Cluster headaches can occur at any time of the day, but typically take place or worsen in fall or spring months (during season changes). Cluster headaches can last for days or months, and then go into remission, so a person doesn’t experience them for quite some time.
Advertisement
Cluster headaches affect one in every 1,000 people and occur in men more than women. A person who suffers from cluster headaches can experience them up to three times a day. Continue reading…
 Migraines don’t solely affect patient, takes toll on spouse, too
Migraines don’t solely affect patient, takes toll on spouse, too
Migraines are exceptionally painful for the sufferer, but they can also take a toll on the patient’s spouse, too. A new study reports that the spouses of migraine sufferers are more likely to suffer from migraines as well. Lead author Dawn Buse said, “This study highlights the significant burden that migraine can have on a wide range of family activities, parenting responsibilities, spousal relationships, and family finances.” The researchers surveyed nearly 4,000 migraine sufferers and spouses.
Over two of every five migraine sufferers and 23 percent of spouses report that the migraine sufferer would be a better parent if they did not live with the condition. Nearly half of migraine sufferers have missed at least one family event as a result of migraines within the last month. Continue reading…
