August is National Immunization Awareness Month, so we share a selection of our articles explaining the importance and effectiveness of immunization, along with new developments, with regards to fibromyalgia, rheumatoid arthritis, shingles, influenza, and norovirus.
Vaccination and immunization are important to help ward off illness. For example, the annual flu shot can help lower your risk of developing the illness, which could potentially be lifesaving if you are in a high-risk group for complications.
Advertisement
During the month of August, we discuss the importance of immunization in the wake of the upcoming fall season and back-to-school time, reminding the families to stay up-to-date on their vaccination schedules.
If you already have a pressing medical condition, you may wonder if getting immunized is safe for you. Information in the articles below – and a consultation with your doctor – should clear this up.
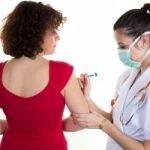 In fibromyalgia patients, influenza vaccination is safe and effective: Study
In fibromyalgia patients, influenza vaccination is safe and effective: Study
Influenza vaccination is safe and effective for fibromyalgia patients. The flu shot is widely recommended by many health authorities as a means of preventing influenza, as it sometimes can contribute to life-threatening consequences. It has been questioned whether the flu shot could cause or exacerbate fibromyalgia. The study evaluated the effectiveness of the flu shot in 19 fibromyalgia patients along with 38 healthy individuals.
The researchers concluded that the flu shot is not only safe but effective, too, in fibromyalgia patients, similarly to its effectiveness in other conditions like rheumatoid arthritis.
The authors concluded, “Despite debate in the literature regarding the role of vaccinations in many connective tissue disorders, vaccinating FMS [fibromyalgia syndrome] patients against influenza is both safe and effective.” Continue reading…
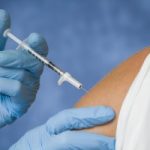 Rheumatoid arthritis patients missing influenza and pneumonia vaccinations face high infection risk: New study
Rheumatoid arthritis patients missing influenza and pneumonia vaccinations face high infection risk: New study
Rheumatoid arthritis (RA) patients missing influenza and pneumonia vaccinations face a higher risk of infection, according to research. The researchers looked at data from over 15,000 patients diagnosed with rheumatoid arthritis who were treated with some types of immunosuppressive medications. At least one in five patients were not vaccinated for influenza, and one in two patients were not vaccinated for pneumonia.
Patients with rheumatoid arthritis have a heightened risk for infection, so vaccination guidelines should be utilized in order to reduce the risk of harmful infections in these patients.
Lead researcher Dr. Will Dixon said, “There is no national data on vaccination uptake broken down in a way that allows us to pull out those with RA. Only one study in the US has looked at whether patients with rheumatic diseases are being vaccinated prior to starting immunosuppressive therapy.”
Dr. Ben Brown, who was also part of the study, added, “Guidance on influenza and pneumococcal vaccination for RA patients is unclear, and payment to carry it out in primary care is variable. In future, it may be beneficial for rheumatologists to provide GPs with specific advice about appropriate vaccination for individual patients, or to consider administering the vaccinations themselves in their own clinics – either way, both approaches should be adequately funded.”
Richard Francis, head of research liaison and evaluation at Arthritis Research U.K., said, “Around 400,000 people in the U.K. live with the excruciating pain of rheumatoid arthritis. The impact of rheumatoid arthritis and the drugs used to treat the condition on the ability to fight infection is significant, and this study underscores the importance of vaccination in helping prevent the impact of influenza and other infections.” Continue reading…
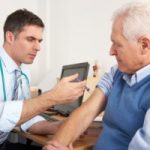 Shingles vaccine safe for rheumatoid arthritis patients taking biologic drugs
Shingles vaccine safe for rheumatoid arthritis patients taking biologic drugs
Shingles vaccine is safe for rheumatoid arthritis (RA) patients taking biologic drugs. Shingles occurs in one in three U.S. adults, with age being a large factor. This is why the vaccine is recommended for those over the age of 50. Rheumatoid arthritis is an autoimmune disease in which the joints are attacked, resulting in stiffness and swelling usually in smaller joints. An estimated 1.3 million Americans live with rheumatoid arthritis and women are twice as likely to develop the condition.
Previously, the shingles vaccine was not recommended for rheumatoid arthritis patients taking biologic medications, but the recent study has shown it to be safe. The researchers studied the safety of the shingles vaccine among 176 rheumatoid arthritis patients who were on either infused or subcutaneous biologics.
Lead author Dr. Stephen Lindsey said, “Every month, I see patients with RA who have had shingles. Despite having an effective vaccine since 2006, our CDC and ACR guidelines do not recommend using it in rheumatic patients on biologics. Studies in 2011 and 2012 suggested no increase in zoster complications inadvertently receiving [herpes zoster] vaccine. We decided to develop and test a protocol to safely vaccinate high-risk patients and help prevent zoster and its complications.”
Eighty percent of infused biologics patients and 50 percent of subcutaneous biologics patients were vaccinated, and no patients developed shingles within six weeks after vaccination. Since 2012, three patients in the infused group and one in the subcutaneous group developed herpes within 10 to 20 months, but no patients developed complications.
Dr. Lindsey added, “Using this protocol, there have been no occurrences of herpes zoster post-vaccination. I feel we can begin to safely vaccinate the thousands of patients who have been on biologics for years and are presently unvaccinated and at high risk.” Continue reading…
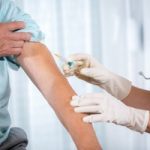 Flu vaccine stops influenza and lowers heart attack and stroke risk
Flu vaccine stops influenza and lowers heart attack and stroke risk
Led by Jacob A. Udell, M.D., M.P.H., F.R.C.P.C., the researchers from the University of Toronto looked at five published randomized placebo-controlled trials (RCT) and one unpublished RCT that had investigated the influenza vaccine and cardiovascular events. Their goal was to determine if the flu vaccine lowers the risk of cardiovascular conditions, such as heart attack. In total, 6,735 patients with an average age of 67 were included in the study. Fifty-one percent of these patients were women, and 36 percent of patients had a history of cardiovascular problems.
From the five published studies, 95 out of 3,238 patients (2.9 percent) that received the influenza vaccine suffered from a major cardiovascular event during the one-year follow-up period. In contrast, 151 out of 3,231 patients (4.7 percent) who received a placebo or control treatment suffered from a major cardiovascular event during the one-year follow-up period. Continue reading…
 Norovirus vaccine, world’s first human clinical trial initiated by Takeda, outbreak reported among GOP convention staffers
Norovirus vaccine, world’s first human clinical trial initiated by Takeda, outbreak reported among GOP convention staffers
Norovirus update 2016: A norovirus vaccine development is underway, with the world’s first human clinical trial initiated by Takeda, one of the top pharmaceutical companies. Meanwhile, a norovirus outbreak has been reported among GOP convention staffers.
Takeda has begun human trials for their norovirus vaccine. There is currently no proper treatment nor vaccine for the virus, which is quite difficult to replicate in the lab setting for proper examination.
Advertisement
The most common form of gastroenteritis, norovirus is responsible for estimated 700 million hospital visits every year. Symptoms include vomiting, diarrhea, and abdominal cramping. Patients usually recover from the virus within a few days, but in severe cases it can lead to dehydration and hospitalization.
Norovirus is highly contagious and can be transmitted through contaminated food or contact with an infected person.
The Takeda trial will include 3,400 persons and will take place in August 2017. The vaccine will be compared to a placebo in a healthy control group recruited from the U.S. military training installations.
Robert Goodwin, head of norovirus development at Takeda, said, “This trial moves us one step closer to putting an important tool for prevention in the hands of individuals, families, and public health systems around the globe.” Continue reading…
