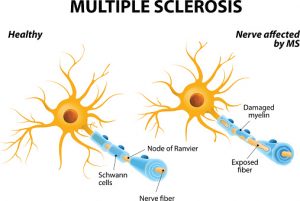
 Multiple sclerosis paroxysmal symptoms can be confused with seizures due to its sudden onset. Paroxysmal symptoms are unique to multiple sclerosis (MS) and involve unusual sensations or muscular contractions. The main differences between multiple sclerosis paroxysmal symptoms and epileptic seizures are that paroxysmal symptoms do not cause short-circuiting of brain waves and do not have other features in the brain, such as epileptic seizures.
Multiple sclerosis paroxysmal symptoms can be confused with seizures due to its sudden onset. Paroxysmal symptoms are unique to multiple sclerosis (MS) and involve unusual sensations or muscular contractions. The main differences between multiple sclerosis paroxysmal symptoms and epileptic seizures are that paroxysmal symptoms do not cause short-circuiting of brain waves and do not have other features in the brain, such as epileptic seizures.
Paroxysmal symptoms can be sudden but are short lasting, and if symptoms last for several days, it could be due to exacerbation or relapse. There are many conditions and symptoms that can trigger paroxysmal symptoms, including fatigue, change in temperature, emotional changes, or a sudden change in body position.
Types of paroxysmal symptoms in MS
Advertisement
Many symptoms of multiple sclerosis can appear and disappear. Here are the most common ones:
 Diplopia: double vision caused by weakness in muscles that control the eyes
Diplopia: double vision caused by weakness in muscles that control the eyes- Paresthesia: abnormal sensations described as burning, tingling, prickling, itching, numbness or pins and needles
- Trigeminal neuralgia: intense pain occurring in the lower part of the face
- Ataxia: unsteadiness or lack of coordination
- Dysarthria: speech disorder where pronunciation is unclear, even when the meaning of what is said is correct
- Pain
- Weakness
- Pruritus: severe itchiness
- Akinesia: being unable to move
- Seizures
- Dystonia: impaired or disordered muscle tone that slows movement or extended muscle spasm
These symptoms typically do not last long, but in the moment they can become quite severe. Unfortunately, paroxysmal symptoms can reoccur or happen several times throughout the day. Medications can be prescribed in order to control them.
Paroxysmal symptoms not to be confused with MS seizures
Seizures can occur in those with multiple sclerosis, and it’s estimated that they affect two to five percent of patients. Similar to paroxysmal symptoms, seizures, too, have a sudden onset, which is why the two conditions can be confused.
 Common seizures that can occur in MS patients include:
Common seizures that can occur in MS patients include:
- Generalized tonic-clonic seizure – brief episode of unconsciousness and uncontrollable movement
- Generalized absence seizures – momentary lapse of consciousness without abnormal movement
- Partial complex seizures – episodes of stereotyped repetitive movement where a person appears awake but does not respond
Treatment of paroxysmal symptoms in MS
There are many triggers that can cause paroxysmal symptom, so by identifying triggers you can reduce the risk of experiencing them. For example, moving your body into a certain position or being too hot can trigger paroxysmal symptoms. Avoiding such situations could reduce their frequency.
There may also be triggers that you are not aware of, so it is useful to keep a diary or make note of when episodes of paroxysmal symptoms occur. You can track settings, movements, foods, or anything else that may have occurred prior to the episode so you can avoid it in the future.
Speaking to your doctor is also important for treatment; they can offer medications for specific symptoms.
It’s important to note that experiencing paroxysmal symptoms does not indicate an MS relapse or that multiple sclerosis is worsening. Paroxysmal symptoms occur due to stimulation. For the best treatment, it’s important to identify triggers and stimulants for better control.
Related Reading:
Multiple sclerosis and the prevalence of sleep disorders, epileptic seizures
Sleep disorders and epileptic seizures are of higher prevalence in those with multiple sclerosis. Multiple sclerosis is a chronic disease that affects the nervous system. Multiple studies have shown higher prevalence of other co-morbid disorders in those with multiple sclerosis, including sleep disorders and epileptic seizures. Continue reading…
Advertisement
Multiple sclerosis patients receive help with safe form of estrogen
Relapse-remitting multiple sclerosis (RRMS) patients taking a safe form of estrogen – estriol – along with conventional medications avoided relapse according to a recent UCLA clinical trial. Researchers made observations at the bedside, tested them in labs and brought back the findings to the patients. Continue reading…
Sources:
https://multiplesclerosis.net/symptoms/paroxysmal-symptoms
http://ms.about.com/od/signssymptoms/a/paroxysmal_utd
http://msfocus.org/article-details
http://www.nationalmssociety.org/Symptoms-Diagnosis/MS-Symptoms/Seizures
https://www.mstrust.org.uk/a-z/paroxysmal-symptoms#cause
