 Gastroesophageal reflux disorder (GERD) and Barrett’s esophagus (BE) patients have higher rates of obstructive sleep apnea and poor sleep quality. Nearly 20 percent of Americans suffer from GERD, which is chronic heartburn or acid regurgitation. Numerous previous studies have explored the association between GERD and poor sleep quality and have found that GERD patients, on average, have worse sleep, including insomnia, sleep disruptions, and overall low quality of sleep.
Gastroesophageal reflux disorder (GERD) and Barrett’s esophagus (BE) patients have higher rates of obstructive sleep apnea and poor sleep quality. Nearly 20 percent of Americans suffer from GERD, which is chronic heartburn or acid regurgitation. Numerous previous studies have explored the association between GERD and poor sleep quality and have found that GERD patients, on average, have worse sleep, including insomnia, sleep disruptions, and overall low quality of sleep.
Research has also shown that GERD is a factor for obstructive sleep apnea (OSA), which is a sleep disorder characterized by the stoppage of breathing throughout the night. GERD may contribute to sleep apnea by causing upper airway inflammation from occurring, but sleep apnea may lead to GERD, because it causes an increase in intra-thoracic pressure.
OSA and poor sleep quality more frequent in GERD, but not BE
Advertisement
To uncover the association between GERD, BE, and poor sleep, researchers conducted a case-controlled study with an ongoing cross-sectional study of BE risk factors. Eligible patients, who were scheduled for an elective upper endoscopy, were recruited. Patients eligible for a colonoscopy underwent an endoscopy along with a colonoscopy, too. Researchers also collected self-reported data with regards to GERD symptoms, sleep quality, and risk of sleep apnea along with the endoscopy findings.
The researchers found that obstructive sleep apnea cases were higher among GERD patients as opposed to Barrett’s esophagus patients, when compared to the controls. Poor sleep quality was also higher in GERD patients than BE patients. Even when other factors that can contribute to poor sleep – smoking, BMI, hypertension, to name a few – were accounted for, the rates of poor sleep were still higher in the GERD group than the BE group and the controls.
Barrett’s esophagus is considered a more severe condition than GERD, and yet the researchers found that poor quality and sleep apnea were more closely associated with GERD than Barrett’s esophagus.
Another study states obstructive sleep apnea is a risk factor for Barrett’s esophagus
Although the above study did not find that Barrett’s esophagus is a risk factor for sleep apnea, an alternative study found that sleep apnea may increase the risk of Barrett’s esophagus.
Both sleep apnea and Barrett’s esophagus share common risk factors, including being overweight or obese, and having GERD. For this study, data was collected from the Mayo Clinic databases and categorized into four groups: Barrett’s esophagus patients with no sleep apnea, sleep apnea patients with no Barrett’s esophagus, patients having both conditions, and patients having neither condition.
Patients with sleep apnea were 80 percent more likely to develop Barrett’s esophagus, compared to patients without sleep apnea. The results remained unchanged even after factoring in smoking, BMI, GERD, age, and sex. Furthermore, the greater the severity of sleep apnea was, the higher the risk of Barrett’s esophagus was.
GERD and sleep apnea treatment options
 Some treatment options can work to improve both sleep apnea and GERD simultaneously, while others are more specific to a particular condition. Treatment options for GERD and sleep apnea include:
Some treatment options can work to improve both sleep apnea and GERD simultaneously, while others are more specific to a particular condition. Treatment options for GERD and sleep apnea include:
- Losing weight, which is a factor for both GERD and sleep apnea
- Taking heartburn medication
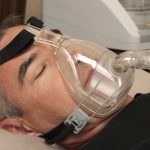
- Using CPAP device – a face mask worn at night to help treat sleep apnea
- Being mindful of what you eat – some foods trigger more acid than others
By working closely with your doctor – you may require two, one for GERD and a sleep specialist for sleep apnea – you can better control and treat both conditions.
Related Reading:
Sleep apnea treatment reduces readmission of heart failure patients
Treatment of sleep apnea may reduce six-month readmission of heart failure patients. First author Sunhil Sharma said, “Our research showed that early recognition and treatment of patients hospitalized with decompensated congestive heart failure is associated with a reduction in readmissions, for patients who use their positive airway pressure (PAP) therapy on a regular basis. Importantly, hospitals can implement cost-effective screening programs to catch sleep apnea in hospitalized, high-risk patients.” Continue reading…
Advertisement
Scleroderma, a GERD risk due to excess collagen in esophagus
Scleroderma is a gastroesophageal reflux disease (GERD) risk due to excess collagen in the esophagus. Scleroderma (systemic sclerosis) is a condition involving a group of diseases that result in the hardening of the skin and connective tissues. Typically, scleroderma affects just the skin, but in some individuals it can also affect structures of the body like blood vessels, causing them to harden. Continue reading…
Sources:
http://onlinelibrary.wiley.com/doi/10.1111/nmo.12265/pdf
http://www.cghjournal.org/article/S1542-3565(13)01300-1/abstract
http://www.everydayhealth.com/gerd/sleep-apnea-and-gerd.aspx
