 Connection between chronic spontaneous urticaria (CSU) and parasite infections (PI) has been found through analysis. The association has been suggested for more than 65 years, but the latest exhaustive review revealed parasite infections in CSU. The findings were published in Allergy.
Connection between chronic spontaneous urticaria (CSU) and parasite infections (PI) has been found through analysis. The association has been suggested for more than 65 years, but the latest exhaustive review revealed parasite infections in CSU. The findings were published in Allergy.
In nearly 90 percent of CSU cases, there is no known cause ever found, which makes the findings so significant. Some potential underlying causes for CSU are food intolerances, autoimmunity, and infections.
Advertisement
The review consisted of 39 studies that found the prevalence of parasite infections in adult and pediatric patients to be zero to 75.4 percent. The authors wrote, “CSU patients were more often diagnosed with protozoa, had a significantly higher risk of toxocariasis seropositivity and Anisakis simplex sensitization, when compared to healthy controls.”
In the reviewed studies, different methodologies were used, including stool examinations, serology, blood eosinophil counts, skin prick tests, and duodenal fluid aspiration.
Treatment for parasite infections varied as well across the reviewed studies from antiparasitic drugs to fish-free diets.
The authors observed, “Analyzing the available data, we can conclude that PI is an uncommon underlying cause of CSU. PI should only be regarded as the underlying cause of CSU when the treatment of parasitosis led to the eradication of the parasite and the remission of CSU. Concurrent GI [gastrointestinal] symptoms, a history of previous parasite infections, travel abroad, and unexplained eosinophilia may point to PI in CSU patients. Further studies are needed to determine the prevalence of CSU in PI and vice versa, and better characterize underlying pathomechanisms in both diseases.”
Chronic hives (urticaria) prognosis and complications
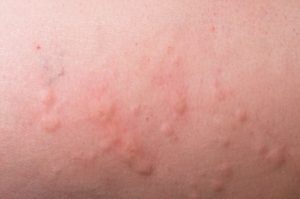
Chronic hives is a condition that can come and go depending on its trigger and cause. In some cases, a rash may be present and then go away. If the rash is severe, it may become itchy, and it can flare up for a variety of reasons, including stress, cold, heat, menstrual cycles, or emotions.
For some, the symptoms may go away for months, even though the condition may stick around for years. In half of the cases of chronic hives, symptoms go away after three to five years, and in one in five cases symptoms come and go over the course of 10 years.
Complications of chronic hives include difficulty breathing and serious allergic reaction. Breathing can become impaired if swelling occurs in the mouth or throat. If this happens, medical attention should be sought out immediately. Anaphylactic shock is also a serous allergic reaction that affects the heart and the lungs. Not only does it impact breathing, but it can result in low blood pressure to the point where a person passes out. Once again, medical attention should be sought out immediately.
Patients who suffer from chronic hives are also at a greater risk for thyroid disease, lupus, rheumatoid arthritis, Sjögren’s syndrome, celiac disease, and type 1 diabetes.
Related Reading:
Chronic hives (urticaria) and penicillin allergy have a strong association: Study
Chronic hives (urticaria) and penicillin allergy have a strong association, according to research. The study found that those living with a penicillin allergy are three times more likely to suffer from chronic hives, compared to the general population. The researchers examined medical records of 11,143 patients, where 220 were identified as having self-reported penicillin allergy and chronic hives. Continue reading…
Advertisement
Chronic hives (urticaria) relief possible with vitamin D: Study
A study has found that vitamin D may offer relief to those living with chronic hives (urticaria). Hives are a reaction of the skin that can be red and quite itchy. There are two types of hives: short-lived (acute) and long-term (chronic). Chronic hives are when the redness and welts last for numerous weeks and come back over the course of months and even years. Continue reading…
Sources:
http://www.hcplive.com/medical-news/connection-between-parasites-and-chronic-spontaneous-urticaria
http://www.ncbi.nlm.nih.gov/pubmed/26648083
http://patient.info/health/chronic-urticaria-hives
http://www.mayoclinic.org/diseases-conditions/chronic-hives/basics/complications/con-20031634
