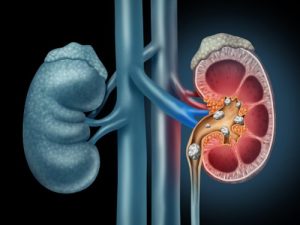
 Calcium oxalate stones are the most common type of kidney stone affecting western society. Kidney stones are abnormal, hard, chemical deposits that form within the kidney, also referred to as nephrolithiasis or urolithiasis. While generally small in size, akin to a grain of rice, some calcium oxalate kidney stones may grow much larger and be difficult to pass.
Calcium oxalate stones are the most common type of kidney stone affecting western society. Kidney stones are abnormal, hard, chemical deposits that form within the kidney, also referred to as nephrolithiasis or urolithiasis. While generally small in size, akin to a grain of rice, some calcium oxalate kidney stones may grow much larger and be difficult to pass.
It is estimated that about 10 percent of people will experience a kidney stone in their lifetime. Of these first-time kidney stone sufferers, about 70 percent will develop recurrences.
How does calcium oxalate stone get formed?
Advertisement
Calcium oxalate kidney stones account for nearly 80 percent of all cases of kidney stones affecting people today. It is a common by-product of human digestion and elimination and usually does not cause us much harm. However, those who are more prone to kidney stone development, as in the case with particular lifestyles and diets, tend to be more likely to develop calcium oxalate stones in the urinary tract.
Eating foods high in calcium cause the minerals to combine with salt of oxalic acid (oxalate) in the large intestine, combining to form calcium oxalate. When this occurs, the new compound becomes less soluble and has difficulty being excreted through the kidney when entering the urinary tract system. While most people have no problems urinating microscopic calcium oxalate crystals, those predisposed to kidney stone development may have problems.
Causes of calcium oxalate stones
We painlessly pass microscopic amounts of calcium, oxalate, phosphate, uric acid, and cystine crystals in our urine all the time. However, when conditions allow these crystals to accumulate and grow in size, it can form bothersome and often painful kidney stones.
The following are some causes of calcium oxalate stones:
Hypercalciuria: Excreting too much calcium in the urine can be a risk factor for kidney stone development. This may be caused by medications like calcium-containing antacids, loop diuretics, and glucocorticoids. Particular medical conditions can also lead to development, as seen with hyperparathyroidism, which is characterized by too much parathyroid hormone; an important factor for calcium regulation in the body. Kidney disease can also lead to high calcium levels in the urine as it is not properly reabsorbed. Additionally, excessive use of vitamin D, an important part of calcium absorption in the gut, may lead to increased calcium levels in the system and increased levels excreted in the urine.
Hyperoxaluria: There are some individuals who are born with a rare genetic variation that causes the excretion of excessive amounts of oxalate in the urine. Consumption of oxalate-rich foods may increase their risk of developing kidney stones. Oxalate-rich foods include beets, chocolate, nuts, rhubarb, spinach, strawberries, tea, and wheat bran. Additionally, it has been known that excessive vitamin C consumption may also lead to increased oxalate levels.
Increased dietary protein: Known to cause increases in both calcium and oxalate levels in the urine, as protein consumption results in lower urinary pH (acidic). Having acidic urine promotes the formation of kidney stones. Acidic enjoinments also decrease citrate levels, a substance is known for helping to minimize kidney stone formation.
Symptoms of calcium oxalate stones
Having kidney stones may not cause any symptoms at all until it moves around your kidney or passes into the ureter, the tube that carries urine from the kidney to the urinary bladder. It is usually at this point when a kidney stone will cause symptoms. The following are some signs that may present in those suffering from calcium oxalate kidney stones:
- Severe pain in the side and back (flank)
- Radiating pain to the lower abdomen and groin
- Pain waves that fluctuate in intensity
- Pain on urination
- Pink, red, or brown colored urine
- Cloudy– or foul-smelling urine
- Nausea and vomiting
- Increased urge to urinate
- Increased frequency of urination
- Fever and chills if an infection is present
- Urinating small amounts
It is advised to seek medical attention if the following signs and symptoms are present:
- Pain with fever and chills
- Bloody urine
- Difficulty passing urine
- Pain so severe that you can’t sit still or find a comfortable position
- Pain accompanied by nausea and vomiting
Who is at risk for calcium oxalate stones?
Certain individuals are more likely to develop kidney stones than others. While some may be due to genetic reasons, most tend to be caused by modifiable lifestyle and dietary habits. The following are some of the most common risk factors for the development of calcium oxalate kidney stones:
- Between the ages of 20 and 40
- Caucasians are more prone than African Americans
- Men are more prone than women
- Having a family history of kidney stones
- Dehydration
- Obesity
- High-protein, salt, oxalate, or glucose diet
- Hyperparathyroidism condition
- Dent disease – a rare disorder affecting the kidneys
- Gastric bypass surgery
- Inflammatory bowel diseases – ulcerative colitis or Crohn’s disease, both conditions lead to improper absorption of fat that binds to calcium, leaving behind excessive amounts of oxalate.
- Taking certain medications – loop diuretics, anti-seizure drugs, and calcium-based antacids.
Prevention of calcium oxalate stones
The following are some of the most commonly recommended calcium oxalate stone treatments and prevention methods. It is important to note that severe or recurrent cases of kidney stones should be looked at by a doctor to better develop a custom-tailored treatment plan, such as finding the most appropriate diet for calcium oxalate stones as well as learning about particular foods to avoid. In any case, what follows is a great way to get a jump start on your kidney stone treatment.
Stay hydrated: The most used method for kidney stone prevention. Drinking plenty of water will help flush out toxins and other substances that may accumulate. Increasing urine volume is the cornerstone of management—most medical professionals recommended an intake of 2.5 to 3 liters of fluids per day.
Don’t decrease calcium intake: While it may make sense to consume less of the substance that contributes to the composition of kidney stones, studies have proven that this does not work. Epidemiologic evidence shows an inverse relationship between dietary calcium intake and recurrence rates. This means that decreasing overall calcium intake can lead to increased kidney stone development. For this reason, low-calcium diets are not recommended for kidney stone prevention.
Limit oxalate-rich foods: Includes rhubarb, dark green leafy vegetables (e.g. Spinach, chard, arugula), beets, wheat bran, nuts, seeds, soy products, chocolate, tea, and strawberries. However, taking these foods with additional fluids and dietary sources of calcium may help diminish oxalate absorption. Additionally, vitamin C can convert to oxalate, so vitamin C supplementation should be taken into account.
Advertisement
Reduce sodium intake: Reductions in dietary sodium is known to reduce calcinuria. It is recommended to reduce sodium intake to less than 2g per day.
Reduce protein intake: Animal protein can have an adverse effect on urinary chemistries, lowering citrate execration and increasing calcium and uric acid excretion. Patients with recurrent stones are advised to minimize protein intake to less than 80g per day.
Related: Essential oils for kidney stones: How to use and recipes
