 What is atheroma?
What is atheroma?
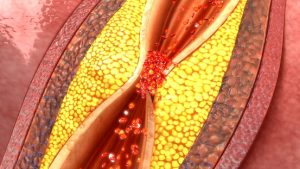
Atheroma refers to small fatty lumps that develop inside blood vessels (arteries). These form as patchy areas of plaque and contribute to the hardening of arteries, a condition known as atherosclerosis.
Atheromas do not develop overnight but instead take months or years to accumulate, becoming larger and thicker. Over time, a patch of atheroma can make an artery narrower, restricting and reducing blood flow through the vessel.
Advertisement
A danger that atheromas exhibit is their tendency to develop tiny cracks or rupture. When this occurs, it can trigger the circulatory system to produce a blood clot (thrombosis) at the site of the atheroma. This can lead to a complete blockage of blood flow at the affected site, potentially causing a heart attack.
What are the causes and symptoms of atheroma?
Atheromas are composed of mostly macrophage cells (a type of white blood cell) or debris, containing lipids (fats), calcium, and a variable amount of connective tissue. When these materials accumulate, they lead to the narrowing of the artery they are attached to. Atheromas do not occur in veins, the blood vessels responsible for delivering de-oxygenated blood back to the heart, as they are not subjected to the same hemodynamic pressure that the arteries are.
Arteries are composed of multiple layers of tissue, and atheromas can accumulate in the tunica intima layer that is between the endothelium lining and the smooth-muscle middle layer of the artery wall.
The most important contributors to endothelial dysfunction or damage are hemodynamic disturbances (high blood pressure), hypercholesterolemia (high cholesterol levels), and inflammation. Toxins that originate from cigarettes, homocysteine, and wide-spectrum infectious agents may also contribute to atheroma development.
However, the exact origins of atheromatous plaque are not well understood. These fatty streaks can be found in the artery walls of infants but are usually absorbed. But in certain cases, incomplete absorption may contribute to atheromatous plaque later in life.
Signs and symptoms of atheromas include:
- Angina (chest pain)
- Breathlessness
- Heart attack
- Stroke
- Transient ischemic attack (TIA)
- Peripheral vascular disorder
- Vascular dementia
- Pain in the calf
- Abdominal pain
- Nausea
Effects of atheroma
Atheromatous plaque causes partial or complete obstruction of an artery. In the majority of cases, a clot formation is responsible for complete blockage. Commonly, the extent of ischemic damage depends on the size of the artery involved and whether collateral circulation is present to help bypass the blocked artery. Often the arteries of the heart, abdomen, and pelvis are affected by atheromatous plaque. Effects of atheromas include:
- Narrowing of an artery: This results in an incomplete supply of blood to the affected tissue found beyond the site of the blockage. The cells of the tissue may be able to perform at a lower capacity, but during times of increased use, such as when muscle activity is greater, pain in the form of cramping may occur. The pain can be relieved by rest. When this phenomenon involves the heart muscles, it is called angina pectoris.
- Occlusion of an artery: This is the complete blockage of an artery and it leads to cellular death due to a lack of blood supply. When this occurs, it is called infarction. If this phenomenon occurs in a major vessel in the heart, it can lead to a myocardial infarction or heart attack, which often results in severe disability or even sudden death.
Complications of atheroma
Atheromas and the narrowing or complete blockage of arteries can lead to several complications. When the fibrous cap covering plaque breaks down, platelets involved in blood clot formation become activated. When enough platelets reach the site of the plaque, a blood clot forms, causing ischemia and infarction.
Additionally, if atheromatous plaque becomes calcified, it makes the artery brittle, rigid, and unresponsive to increases in blood pressure. This can result in a ruptured artery, leading to a hemorrhage or excessive bleeding. Another potential complication can occur due to weakened arterial walls caused by plaque that has developed between layers of blood vessel tissue. This may lead to an aneurysm, which is an enlargement of part of the artery, and there is a chance the artery could rupture.
Advertisement
Additional complications of atheromatous plaque include:
- Heart disease and heart attack.
- Cerebrovascular disease such as TIA and stroke, which can lead to brain damage.
- Peripheral arterial disease, which, due to narrowing of arteries in the leg, commonly leads to cramps and muscle pain.
- Vascular dementia, the second-most common variety of dementia after Alzheimer’s disease. Reduced blood supply damages the regions of the brain involved in memory and cognition.
Preventing atheroma
Several factors that contribute to atheromatous plaque formation can be effectively thwarted. They are referred to as modifiable risk factors.
- Smoking: A strong risk factor for vascular disease as it causes blood vessel constriction, which raises blood pressure, and platelet activation.
- Diet and exercise: A poor diet and lack of exercise may lead to obesity, which is partly responsible for the development of high blood pressure. A greater prevalence of sedentary behavior has caused obesity rates to reach record-high levels, increasing the risk for diseases related to atherosclerotic plaque.
- Dyslipidemia: This is an abnormal amount of lipids in the blood. It is often caused by a combination of genetic and dietary factors. Modern medical science has linked a lower total plasma cholesterol concentration with a reduction in coronary heart disease. Diets typically focus on reducing saturated fat and correcting obesity.
Related: 10 foods to help prevent clogged arteries naturally
