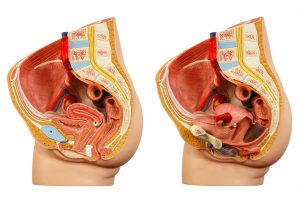
 Pelvic organ prolapse risk raises with high body mass index (BMI) after pregnancy. Having a healthy BMI has been associated with overall good health, but having your BMI in the unhealthy range increases the risk of a number of various health issues, including heart problems – and organ prolapse. Maintaining a healthy BMI may also help prevent prolapsed pelvic organs, especially after pregnancy.
Pelvic organ prolapse risk raises with high body mass index (BMI) after pregnancy. Having a healthy BMI has been associated with overall good health, but having your BMI in the unhealthy range increases the risk of a number of various health issues, including heart problems – and organ prolapse. Maintaining a healthy BMI may also help prevent prolapsed pelvic organs, especially after pregnancy.
The study looked at 108 women from China and evaluated the role of BMI in pelvic organ prolapse. Lead researcher Dr. Marsha K. Guess said, “We found that an important risk factor for prolapse for women one year after delivery was their BMI, regardless of their baseline BMI at the first trimester, or how much they gained during pregnancy. Specifically, the higher the BMI one year after delivery, the higher the risk for having pelvic floor laxity and increased odds for early stage pelvic organ prolapse.”
Advertisement
Nearly 50 percent of women over 40 who have given birth vaginally will experience pelvic organ prolapse, which can lead to bladder problems and poor bowel control.
Although previous studies have shown that higher BMI in non-pregnant women increases the risk of organ prolapse, this study stresses the importance of maintaining a healthy BMI after delivery in order to lower the risk of organ prolapse.
Guess continued, “Our findings show that even small differences in BMI one year after delivery can lead to pelvic floor laxity in normal-weight women. These results shed light on a potential critical, time-dependent opportunity to modify the risk of developing pelvic organ prolapse for some women. Getting women into a routine of healthy diet and exercise habits, and back to their baseline weight after delivery may play an important role in preventing the early stages of prolapse.”
Treatment for pelvic organ prolapse
Treatment choice for pelvic organ prolapse depends on the severity of symptoms, the severity of prolapse, patient’s age and health status, as well as plans on having children in the future.
If organ prolapse is mild or moderate, treatment may not be necessary, but if you experience pain and discomfort, your doctor will recommend some form of therapy.
Treatment for prolapsed pelvic organs can vary from at-home lifestyle changes to medical interventions. Treatment options include performing pelvic floor exercises, losing weight, eating a high-fiber diet, avoiding heavy lifting, starting hormonal replacement therapy, using a vaginal pessary (a device inserted into the vagina to hold back the prolapsed organ), and lastly, going for surgery.
Advertisement
Your surgeon will try to repair the prolapsed organ and put it back into place. In some cases, a vaginal mesh is inserted to support the prolapsed organ. There are plenty of risks and side effects associated with surgical intervention, so it’s important that you speak with your doctor to understand the risks you are facing and to make an informed decision.
Based on your case, your doctor will be able to assess which option is right for you to treat your pelvic organ prolapse.
Sources:
http://news.yale.edu/2015/10/26/high-post-pregnancy-bmi-raises-pelvic-organ-prolapse-risk
//www.belmarrahealth.com/prolapsed-bladder-cystocele-causes-symptoms-surgery-treatments/
