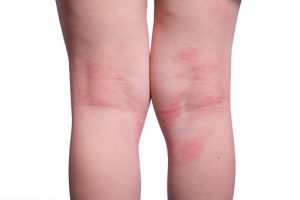
 Shingles and eczema are skin conditions that can cause a rash-like appearance and inflammation of the skin. Knowing the differences between the two can aid in proper diagnosis as both require a specific treatment.
Shingles and eczema are skin conditions that can cause a rash-like appearance and inflammation of the skin. Knowing the differences between the two can aid in proper diagnosis as both require a specific treatment.
Shingles is a painful rash that is commonly seen among seniors. It is caused by the herpes zoster virus and can appear anywhere on the body. Shingles is a treatable condition, and there is even a vaccine available for at-risk groups in order to reduce the risk. It’s important that shingles is caught early as it can lead to serious health complications.
Advertisement
Eczema refers to a non-contagious skin condition, which causes the skin to become inflamed, red, dry, and itchy. The exact cause isn’t well understood, but there are many factors that may trigger its onset.
Here we will outline the symptoms, causes, and treatments for both shingles and eczema to help you spot these conditions and understand how to treat them.
Shingles vs. eczema: U.S. prevalence
Roughly 31.6 million Americans have eczema, with 17.8 million living with the severe eczema. Prevalence of eczema can range from 10.7 to 21 percent across the U.S., depending on the state.
One in three Americans will develop shingles in their lifetime, and the risk of shingles goes up after the age of 50. Roughly one to four percent of shingles patients will be hospitalized for shingles-related complications. These individuals tend to have weakened immune systems.
Ninety-six people die of shingles annually, and deaths are common among senior patients or those with weakened immune systems. There has been a steady incline of shingles cases, though the reason behind this trend is unclear. One theory suggests that less people are exposed to the virus due to the decline of chickenpox cases. As a result, less people are building immunity against it.
Comparing shingles and eczema: Signs and symptoms
 Signs and symptoms of eczema include dry and sensitive skin, intense itching, skin redness and inflammation, recurring rash, scaly areas, rough leathery patches, oozing and crusting of the skin, areas of swelling, and dark colored patches on the skin.
Signs and symptoms of eczema include dry and sensitive skin, intense itching, skin redness and inflammation, recurring rash, scaly areas, rough leathery patches, oozing and crusting of the skin, areas of swelling, and dark colored patches on the skin.
Symptoms of shingles include pain, burning, numbness or tingling of the skin, sensitivity to touch, a red rash followed by days of pain, fluid-filled blisters that break open and crust over, and itching. Some patients may experience fever, headache, sensitivity to light, and fatigue.
You should see a doctor immediately if the shingles rash is near the eyes, as it can lead to permanent eye damage if you are over the age of 70, if you have a weakened immune system, or if the rash is widespread and painful.
Difference between shingles and eczema causes
Shingles is caused by the varicella zoster virus, which is the same virus that causes chickenpox. If you have previously had chickenpox, there is a higher risk of having shingles later on in life. Even if you’ve recovered from chickenpox, the virus can be dormant and remain in the nervous system. Throughout the years, the virus can become reactivated and present itself as shingles.
The reason why the varicella zoster virus reactivates is unclear and may have to do with aging and a weakened immune system, hence the prevalence of shingles among older adults.
The exact cause of eczema is unknown. Because it often resembles an allergy, researchers believe that environmental factors may trigger the condition. A combination of factors may come into play with regards to the cause of eczema, including genetics, abnormal functioning of the immune system, environment, activities that cause the skin to be more sensitive, and defects in the skin barrier allowing moisture out and germs in.
Eczema has been found to run in families, so heredity may be a contirbuting factor. It is also more common in asthma patients and in those who suffer from allergies.
Are shingles and eczema contagious?
 Shingles is highly contagious to those who are not immune to the virus. Shingles can be transmitted through direct contact with sores, but a person who contracts shingles from an affected person will develop chickenpox, not shingles.
Shingles is highly contagious to those who are not immune to the virus. Shingles can be transmitted through direct contact with sores, but a person who contracts shingles from an affected person will develop chickenpox, not shingles.
If you have shingles, in order to reduce transmission of shingles to others, ensure your rash is well covered, avoid scratching and touching the rash, wash your hands often, and avoid contact with at-risk people like pregnant women, those with weakened immune systems, individuals undergoing cancer treatment, and premature or low-weight babies.
Eczema, on the other hand, is not contagious and cannot be passed on from person to person. It is important to note if the rash becomes infected then the infection is contagious.
Eczema vs. shingles: Risk factors and complications
Risk factors for shingles include being over the age of 50, having certain diseases especially those that weaken the immune system like HIV, undergoing cancer treatment, and taking certain medications, such as steroids or medications that prevent transplanted organs from being rejected.
If left untreated, shingles can result in complications including post-herpetic neuralgia, where the pain persists long after shingles has been cleared up, vision loss if the rash is near the eye, neurological problems, facial paralysis, hearing or balance problems, and skin infections.
Risk factors for eczema include genetic factors – such as having parents who suffer from allergies, asthma, and hay fever, environmental factors – like skin irritants, extreme temperatures, and lack of moisture after bathing, as well as medical conditions – like asthma and allergies. Other at-risk groups are infants as the majority of eczema cases occur within the first year of life, and overweight individuals, as obesity can worsen eczema.
Complications related to eczema include asthma and hay fever, chronic itchy and scaly skin, skin infections, irritant hand dermatitis, allergic contact dermatitis, sleep problems, behavioral problems, and eye problems like watering, itchy eyes and inflammation of the eyelid.
Differentiating shingles and eczema: Diagnosis and treatment
 Shingles is diagnosed through examining the history of pain on one side of the body and the appearance of a rash and blisters. Your doctor may take tissue samples of the blisters for laboratory examination to confirm diagnosis.
Shingles is diagnosed through examining the history of pain on one side of the body and the appearance of a rash and blisters. Your doctor may take tissue samples of the blisters for laboratory examination to confirm diagnosis.
Treatment of shingles is done with prescribed antiviral medications, which include acyclovir, valacyclovir, or famciclovir. Along with antivirals, your doctor may also recommend other treatments to ease symptoms, including capsaicin cream, anticonvulsants, antidepressants, numbing agents, medications that contain narcotics, and corticosteroid injections.
Eczema is easily recognizable, so after examining the rash and reviewing the patient’s medical history, a doctor will be able to diagnose eczema. Your doctor may perform some testing to ensure it is not another condition.
It may take several different treatments to properly treat eczema, as the rash can be persistent. As long as it is caught early, treatment can begin right away. Some treatments for eczema include creams for itching and inflammation, creams for skin repair, drugs to fight off infection, oral anti-itch drugs, and oral or injected drugs to control inflammation.
Some therapies for eczema treatment include wet dressings, light therapy, stress treatment and relaxation, as well as behavior modification, or biofeedback, which can help treat habitual scratching.
If you have eczema, you will also want to avoid skin irritants like perfumes or wool, avoid extreme temperatures, and use lotions and oils regularly to keep your skin moist.
Related Reading:
Shingles-related chronic pain – known as neuropathic pain – caused by nerve damage can be treated with a new drug. This drug may also be able to combat neuropathic pain experienced in HIV, diabetes, nerve injury, and cancer chemotherapy. Continue reading…
Advertisement
Eczema-like inflammation caused by staph bacteria (staphylococcus aureus) infection
Eczema-like inflammation is caused by staph bacteria (staphylococcus aureus) infection. Eczema is a skin condition that leads to red, itchy rashes with no known cause. Researchers from the University of Michigan Medical School have now brought the medical community one step closer to better understanding of eczema with hopes to help improve treatments. Continue reading…
Sources:
http://www.cdc.gov/shingles/surveillance.html
https://nationaleczema.org/eczema/symptoms/
http://health.cvs.com/GetContent.aspx?token=f75979d3-9c7c-4b16-af56-3e122a3f19e3&chunkiid=19380
