 According to new research, patients with peripheral artery disease (P.A.D.) or stroke are less likely to receive recommended treatments to prevent heart attack. The study comes from American Heart Association’s Quality of Care & Outcomes Research Scientific Sessions, which is a premier global exchange of the latest advances in the quality of care and research in cardiovascular disease and stroke.
According to new research, patients with peripheral artery disease (P.A.D.) or stroke are less likely to receive recommended treatments to prevent heart attack. The study comes from American Heart Association’s Quality of Care & Outcomes Research Scientific Sessions, which is a premier global exchange of the latest advances in the quality of care and research in cardiovascular disease and stroke.
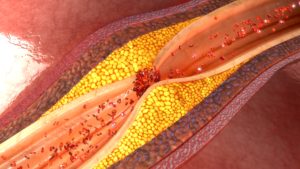
Cardiovascular disease is the leading cause of death worldwide, and the main contributing factor is atherosclerosis. This is the condition that occurs when cholesterol, fat, and inflammatory cells build up and form plaque that blocks the arteries and impedes blood flow.
Advertisement
Depending on the location of the blockage in arteries, atherosclerosis can increase the risk for three severe conditions, including coronary artery disease, stroke, and peripheral artery disease. Coronary artery disease happens when heart arteries are damaged, which can lead to a heart attack. A common type of stroke occurs when clogged arteries block blood flow to the brain. Peripheral artery disease results from damaged arteries in the extremities. This is most often the legs and can lead to pain during walking and, in severe cases, amputation.
Patients Less Likely to Receive Treatment
During the American Heart Association’s study, researchers found that patients with peripheral artery disease or stroke were less likely than those with coronary artery disease to receive treatments to prevent heart attack.
“Our study highlights the need for public health campaigns to direct equal attention to all three major forms of atherosclerotic cardiovascular disease,” said senior study author Erin Michos, M.D., M.H.S., associate professor of medicine at the Ciccarone Center for the Prevention of Cardiovascular Disease at The Johns Hopkins University School of Medicine in Baltimore. “We need to generate awareness among both clinicians and patients that all of these diseases should be treated with aggressive secondary preventive medications, including aspirin and statins, regardless of whether people have heart disease or not.”
The study compared over 14,000 U.S. adults enrolled in the 2006-2015 Medical Expenditure Panel Survey, a national survey of patient-reported health outcomes and conditions, and health care use and expenses. Just over half the patients were men, the average age was 65, and all had either coronary artery disease, stroke, or peripheral artery disease. These participants were meant to represent nearly 16 million U.S. adults living with one of the three forms of artery-clogging diseases.
Researchers found that compared to participants with coronary artery disease, those with peripheral artery disease were twice as likely to report no statin use. They were also three times more likely to report no aspirin use and had the highest annual out-of-pocket expenditures among the three atherosclerotic conditions. Participants with stroke were more than twice as likely to say no statin or aspirin use and were more likely to report poor patient-provider communication, poor health care satisfaction, and more emergency room visits.
Advertisement
“Our study highlights a missed opportunity for implementing life-saving preventive medications among these high-risk individuals,” Michos said. “Peripheral artery disease and stroke should generally be treated with the same secondary prevention medications as coronary artery disease.”
Since atherosclerosis can affect arteries in more than one part of the body, physicians suggest treating coronary artery disease, stroke, and peripheral artery disease similarly with lifestyle changes and medication, including statins to lower cholesterol levels and aspirin to prevent blood clots.
Many lifestyle changes can go a long way to help reduce the risk of medical implications due to blocked arteries. These include eating a healthy diet, being physically active, quitting smoking, controlling high cholesterol, controlling high blood pressure, treating high blood sugar, and losing weight.
