 Rheumatoid arthritis (RA) and osteoporosis both affect the body skeleton, with the former affecting the joints and the latter making the bones weak and brittle due to bone density loss.
Rheumatoid arthritis (RA) and osteoporosis both affect the body skeleton, with the former affecting the joints and the latter making the bones weak and brittle due to bone density loss.
Osteoporosis affects men and women, but is far more commonly seen among women. In a healthy bone, the tissue is constantly being broken down and replaced, but in osteoporosis the lost tissue is not replaced at the same rate with which the old bone is being broken down. Over time, this can cause fragile bones, increasing a person’s risk for fractures and disability.
Advertisement
Rheumatoid arthritis is an autoimmune disease, which means the body’s immune system begins to wrongfully attack the healthy tissue of the joints. This causes inflammation and pain in the joints, and cartilage begins to wear away. As rheumatoid arthritis becomes more severe, other organs in the body are negatively affected as well, resulting in greater health complications.
Here we will outline the similarities and differences between osteoporosis and rheumatoid arthritis.
Connection between rheumatoid arthritis and osteoporosis
Rheumatoid arthritis affects the joints, while osteoporosis impacts the bones, but unfortunately some treatments intended to help rheumatoid arthritis may contribute to bone loss, thus resulting in osteoporosis. So if you’re wondering – can you have osteoporosis and rheumatoid arthritis together? – the answer is, yes.
Seoyoung C. Kim, a rheumatologist and researcher at Brigham and Women’s Hospital, said, “The bottom line is that people with RA have a high risk of osteoporotic fracture at the typical sites: the hip, forearm, pelvis.” Dr. Kim estimated that the risk of bone fractures is 25 to 30 percent higher in rheumatoid arthritis patients.
Additionally, inflammation associated with rheumatoid arthritis can also contribute to bone damage by stimulating osteoclasts – bone cells that deplete bone minerals. Common treatment for rheumatoid arthritis – corticosteroids – can also contribute to bone mineral loss. Michael DiMuzio, executive director of the North Shore Osteoporosis Center, explained, “Prednisone stops the function of bone-forming cells. When that happens, the body still needs calcium, so it takes it out of the bone, but it’s not allowing the bone-forming cells to put it back.”
Another common treatment for RA, biologics can contribute to the disruption of natural bone remodeling. The good news is, there are newer biologics on the market that do not interfere with this process.
To ensure you are not losing bone density whilst treating your rheumatoid arthritis, it’s important to make the necessary lifestyle changes to promote healthy bones, including getting adequate calcium and vitamins, partaking in weight-bearing exercises, not smoking, reducing alcohol and caffeine intake, and eating an overall healthy diet.
Table: Osteoporosis vs. arthritis
| Osteoporosis | Rheumatoid arthritis | |
| Risk factors | ||
| Age | X | |
| Menopause | X | |
| Family history | X | X |
| Use of some drugs | X | |
| Insufficient calcium | X | |
| Insufficient physical activity | X | |
| Joint overuse | X | |
| Smoking | X | |
| Alcohol consumption | X | |
| Overweight, obesity | ||
| Disease impact on the body | ||
| Bones | X | |
| Joints | X | |
| Autoimmune disease | X | |
| Big or crooked joints | X | |
| Loss of height | X |
Osteoporosis vs. rheumatoid arthritis: U.S. prevalence
An estimated 1.3 million Americans live with rheumatoid arthritis, and women have higher rates of rheumatoid arthritis than men.
In the U.S., 10 million people are affected by osteoporosis and worldwide 200 million people live with this bone disease. Roughly 34 million Americans are at risk for osteopenia – low bone mass – which can contribute to fractures and other complications.
Comparing rheumatoid arthritis and osteoporosis: Signs and symptoms
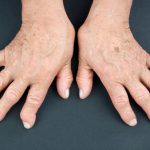 Symptoms of rheumatoid arthritis are often worse in the morning, lasting for about 30 minutes. Swelling occurs symmetrically (both hands, both ankles, etc.).
Symptoms of rheumatoid arthritis are often worse in the morning, lasting for about 30 minutes. Swelling occurs symmetrically (both hands, both ankles, etc.).
Common symptoms in RA include joint pain, swelling, stiffness, tenderness, prolonged morning stiffness, and reduced range of motion. These often occur in smaller joints, such as the hands, can also present themselves in other parts of the body – like skin, eyes, lungs, heart, kidneys, salivary glands, nerve tissue, bone marrow, and blood vessels.
Osteoporosis can be asymptomatic in its early stages, so by the time the symptoms actually begin to present themselves, a significant bone loss could have already occurred.
Symptoms and signs you may begin to notice in osteoporosis include back pain often caused by a fractured or collapsed vertebrae, loss of height over time, a stooped posture, and a bone fracture, which occurs far easier than it should have normally.
Difference between osteoporosis and rheumatoid arthritis causes
Rheumatoid arthritis is a type of an autoimmune disease, but why or how autoimmune diseases occur is still unclear. The immune system mistakes parts of the body for a virus and begins to attack it. In the case of rheumatoid arthritis, the immune system attacks the synovium (a specialized connective tissue).
In osteoporosis, new bone tissue develops much slower than the old tissue is being broken down. In healthy bones, tissue is constantly being broken down and renewed. Over time, this process begins to slow down, so way more tissue is removed compared to new tissue created.
The risk of developing osteoporosis is largely dependent on how much bone mass you accumulated in your younger years. If you stocked up on calcium and vitamin D and exercised regularly, you will have greater bone mass in your “bone bank” than a person who did not partake in these bone-strengthening measures.
Rheumatoid arthritis vs. osteoporosis: Risk factors and complications
 Risk factors for rheumatoid arthritis include:
Risk factors for rheumatoid arthritis include:
- Being a female
- Being over the age of 40
- Family history of RA
- Smoking
- Environmental exposures such as asbestos or silica
- Obesity
Complications that may stem from rheumatoid arthritis include osteoporosis, dry eyes and mouth, infections, abnormal body composition, carpal tunnel syndrome, heart problems, lung disease, and lymphoma.
Risk factors for osteoporosis include:
- Being female
- Older age
- Being white or of Asian descent
- Family history of osteoporosis
- Smaller body frame
- Lower levels of sex hormones
- Thyroid problems
- Overactive parathyroid or adrenal gland
- Low calcium intake
- Low vitamin D
- Inadequate nutrient absorption due to having part of intestine removed
- Eating disorder
- RA, IBS, IBD, kidney or liver disease, lupus, cancer
- Sedentary lifestyle
- Smoking
- Excessive alcohol consumption
One of the complications resulting from osteoporosis is bone fractures that occur far easier than they should, which can contribute to short-term or even long-term disability. Other complications include loss of height and a hunched forward posture.
Differentiating rheumatoid arthritis and osteoporosis: Diagnosis and treatment
Proper diagnosis of rheumatoid arthritis involves a look at the patient’s medical history, symptom review, a physical examination, blood tests to look for antibodies associated with rheumatoid arthritis, and imaging tests to determine any joint damage.
The rheumatoid arthritis treatment aims at reducing inflammation, relieving symptoms, preventing joint and organ damage, improving physical function and well-being, and reducing long-term complications.
Rheumatoid arthritis can be treated with medications to ease symptoms like pain and stiffness. This may involve anti-inflammatory and pain medications. Other medications can be prescribed to slow down the progression of rheumatoid arthritis, including corticosteroids, biologics, and JAK inhibitors. Surgery may be required if damage is severe, and the joint must be replaced in order to improve function.
Osteoporosis is diagnosed by measuring bone density with a machine that utilizes low level X-rays. The test is painless and requires the patient to lay on a padded table while a scanner passes over their body. Primary bones that are tested as a good indication of possible osteoporosis include the hip, wrist, and spine.
Advertisement
Those at an increased risk for bone fractures may get a prescription for medications like Alendronate (Fosamax), Risedronate (Actonel, Atelvia), Ibandronate (Boniva), and Zoledronic acid (Reclast). Unfortunately, as with many medications, these can cause unwanted side effects, too, including nausea and heartburn-like symptoms. As long as medications are taken as directed, you can minimize side effects.
Hormone therapy may also be used to treat osteoporosis, as one of the risk factors for the bone disease is having low sex hormones. Estrogen may help maintain bone density, but it can also come with complications, including the risk of blood clots, endometrial cancer, breast cancer, and possibly heart disease.
There are some alternative remedies for osteoporosis – for example, soy proteins, which act similarly to bone tissue. Some studies have found a reduction in bone fractures among Asian postmenopausal women who consume soy. A word of caution: Soy should be limited or avoided in women with a family history of breast cancer. Speak to your doctor about adding soy into your diet or as a supplement.
Your doctor will help you decide on what type of treatment will offer you the greatest improvement in living with either rheumatoid arthritis or osteoporosis.
