 Osteomalacia is a condition that leads to weakening of the bones. The term itself means “soft bones.” The most common cause of osteomalacia is a vitamin D deficiency. Vitamin D plays an important role in keeping the bones strong as it helps the absorption of calcium.
Osteomalacia is a condition that leads to weakening of the bones. The term itself means “soft bones.” The most common cause of osteomalacia is a vitamin D deficiency. Vitamin D plays an important role in keeping the bones strong as it helps the absorption of calcium.
Although osteomalacia may seem similar to osteoporosis, the two conditions are not the same. Osteomalacia stems from a defect in the process of bone building itself, while osteoporosis is the weakening of the bones that have already been constructed.
Advertisement
Bone fibers are coated with mineral for strength. This process is known as mineralization.
In order for bones to be strong fibers are coated with mineral, this process is known as mineralization. The more coating there is, the stronger the bones will be. When mineralization does not occur properly, although the formation of collagen matrix continues, these fibers are not strengthened with minerals, resulting in soft bones. Soft bones are prone to breaks and fractures, which can lead to disability.
Causes of osteomalacia in older adults
As mentioned, the most common cause for osteomalacia is a vitamin D deficiency. Vitamin D is absorbed through the skin when exposed to sunlight. People living in areas with limited sunlight exposure are at a higher risk of a vitamin D deficiency than those living in sunnier regions.
Undergoing certain types of surgery, such as surgeries on the stomach or intestines, having certain conditions like celiac disease, kidney or liver disorders, and taking certain drugs such as seizure medications may also lead to osteomalacia, as the absorption of essential bone minerals and vitamins becomes limited.
Signs and symptoms of osteomalacia
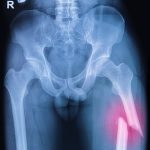 Unlike other bone conditions which are asymptomatic, osteomalacia does present symptoms, such as pain in the bones, muscles weakness, and partial fractures, which are slight cracks in the bones.
Unlike other bone conditions which are asymptomatic, osteomalacia does present symptoms, such as pain in the bones, muscles weakness, and partial fractures, which are slight cracks in the bones.
Bone pain is commonly experienced in the legs, groin, upper thighs, knees, and, sometimes, feet when standing, walking, or running. Sometimes, pain may ease when at rest. Pain may worsen even with the slightest knock to the bone and over time it can intensify with all types of movements.
Diagnosis and tests for osteomalacia
To properly diagnose osteomalacia, the doctor must rule out other conditions and uncover the underlying cause. To diagnose osteomalacia, the patient may be referred for blood and urine tests, X-ray, and a bone biopsy.
Treatment and prevention of osteomalacia
Advertisement
 Although treatment can cure osteomalacia, the patient may continue experiencing symptoms for months. Treatment involves targeting the underlying cause – for example, boosting vitamin D levels, or treating kidney and liver problems.
Although treatment can cure osteomalacia, the patient may continue experiencing symptoms for months. Treatment involves targeting the underlying cause – for example, boosting vitamin D levels, or treating kidney and liver problems.
During treatment, the cracks and minor fractures in the bones will heal, and you can take pain reliever medication to deal with the pain.
Speaking of preventative measures, you need to make sure you’re getting adequate amount of vitamin D by either heading out in the sunlight more (safely, of course) or taking a supplement recommended by your doctor. You can also eat foods rich in vitamin D such as oily fish, egg yolks, or fortified cereals and milk.
