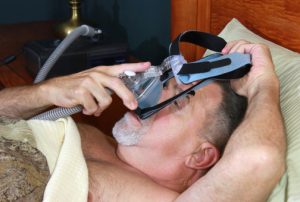
 Obstructive sleep apnea patients with type 2 diabetes see improved glycemic control using CPAP device. Senior study author Dr. Francisco Garcia-Rio said, “[Obstructive sleep apnea] is a public health problem of the first order, due to its high prevalence and marked morbidity and mortality, having been linked to traffic accidents, cardiovascular complications and, more recently, neoplastic diseases. Diabetes mellitus is a global epidemic. There are currently 382 million diabetics worldwide, a figure which is estimated to reach 592 million in 2035.”
Obstructive sleep apnea patients with type 2 diabetes see improved glycemic control using CPAP device. Senior study author Dr. Francisco Garcia-Rio said, “[Obstructive sleep apnea] is a public health problem of the first order, due to its high prevalence and marked morbidity and mortality, having been linked to traffic accidents, cardiovascular complications and, more recently, neoplastic diseases. Diabetes mellitus is a global epidemic. There are currently 382 million diabetics worldwide, a figure which is estimated to reach 592 million in 2035.”
The researchers looked at 50 patients with obstructive sleep apnea and uncontrolled diabetes who were assigned CPAP intervention or served as controls. Diabetes medication was not changed during the study unless it was medically necessary and participants were not requested to change their diet or physical activity levels.
Advertisement
Researchers measured patients’ glucose control, insulin sensitivity and resistance, inflammatory proteins, and other biomarkers seen in type 2 diabetes. Those using CPAP devices had a significant decrease in glycated hemoglobin (HbA1c) levels at three months, an improved insulin at three and six months, and a decrease in insulin sensitivity at six months.
CPAP users also had lower levels of inflammatory markers and higher levels of the hormone adiponectin, an important glucose regulator.
Previous research showed that a one percent decrease in inflammatory markers was associated with a 15 to 20 percent decrease in cardiovascular complications from diabetes.
Dr. Garcia-Rio suggested, “Early identification of OSA in patients with type 2 diabetes, and assessment for metabolic abnormalities in those with OSA could reduce the cardiovascular disease risk of patients with these chronic diseases.”
CPAP machine effective usage tips
Continuous positive airway pressure (CPAP) device is commonly prescribed for individuals with obstructive sleep apnea as it ensures there is a steady airflow, preventing the stoppage of breathing throughout the night which occurs in sleep apnea. The device contains a small machine along with a facial mask, which is worn throughout the night.
Although majority of the time CPAP devices are effective, there are some problems, which may arise and which, fortunately, come with some easy fixes.
The mask is the wrong fit or style: there are many mask types available to choose from that best suit your needs and come in different sizes for the most comfortable fit.
The mask is uncomfortable: you may wish to begin wearing the mask for shorter periods of time and work your way up to sleeping all night with it. You will eventually get used to it and not even notice it’s there.
Trouble adjusting to forced air: many devices allow for different air pressure options, allowing you to start off with low pressure and work your way up.
Dry, stuffy nose: some devices come with a humidifier, and using a nasal saline solution prior to bed can be useful as well.
Feeling claustrophobic: practice using the mask while you’re awake and practice relaxation exercises prior to bed.
Leaky mask, skin irritation, or pressure sores: adjusting the mask and getting a proper size can prevent the mask from leaking, which can cause skin irritation, or causing pressure sores.
Difficulty falling asleep: following proper sleep hygiene can help improve your ability to fall asleep, along with practicing wearing the mask and working your way up gradually to wearing CPAP device all night.
Advertisement
Dry mouth: opting for a full face mask that covers the mouth can prevent dry mouth, or you can wear a chin strap to keep your mouth closed during the night.
Unintentionally removing the mask while asleep: proper fit and wearing a full face mask may prevent you from accidently removing the mask while asleep.
Noisiness: the machine does produce some noise, but many are near silent. If the device is working properly, there should virtually be no noise, but if a noise persists earplugs may offer you relief.
