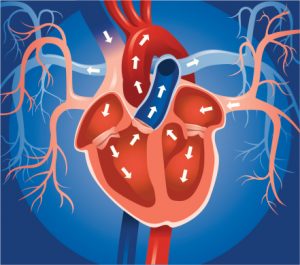
 Left atrial enlargement refers the enlargement of the left atrium and can be the result of many conditions, either congenital or acquired. The left atrium is situated in a way where it receives oxygenated blood sent from the lungs to be pumped into the left ventricle, passing the mitral valve, which is then pumped through them to the rest of the body passing the aortic valve.
Left atrial enlargement refers the enlargement of the left atrium and can be the result of many conditions, either congenital or acquired. The left atrium is situated in a way where it receives oxygenated blood sent from the lungs to be pumped into the left ventricle, passing the mitral valve, which is then pumped through them to the rest of the body passing the aortic valve.
The heart is comprised of four chambers: the right and left atria and the right and left ventricles. All of these chambers work in concert to pump blood into the lungs to become oxygenated and back out to the circulatory system. This is a vital process to ensure that all organs and tissue of your body is provided the necessary oxygen and nutrients needed to perform optimally.
What causes left atrial enlargement?
Advertisement
Left atrial enlargement can be mild, moderate, or severe depending on the severity of the underlying condition. The following are some of the most common congenital and acquired causes of left atrial enlargement.
Acquired
Mitral stenosis
Usually due to an acquired valvular defect resulting in a narrowing of the mitral passage. This is often characterized by the restriction of blood flow from the left atrium to the left ventricle, leading to the development of left atrial enlargement. The most common cause of mitral stenosis is rheumatic heart disease, an inflammatory condition caused by a group A Streptococcus pyogenes infection. However, documented cases of congenital mitral stenosis do exist.
A functional or anatomical dysfunction of the mitral valve causing the leakage of blood backward through the mitral valve as the left ventricle contracts. As a result, the backup of blood into the left atrium increases the pressure within, causing left atrial enlargement as well as increased pressure in the pulmonary veins (leading from the lungs to the heart). Mitral regurgitation can also lead to fluid buildup in the lungs. This condition may be caused by conditions such as a myocardial infarction, infective endocarditis, and Marfan syndrome (a connective tissue disease).
Left ventricular failure
Often called the “workhorse of the heart,” the left ventricle works the hardest of all the chambers in the heart to pump blood to the circulatory system. This is often reflected in its size, being larger than the others. Left ventricular failure is often caused by chronic high blood pressure, coronary artery disease, and faulty heart valves leading to the back up of blood to the left atrium, causing enlargement and other pulmonary symptoms.
Atrial fibrillation (AFib)
An abnormal heart rhythm causing the heart to beat irregularly. While AFib may not always lead to left atrial enlargement initially, over time, it is more likely to develop. If left untreated, AFib may also lead to the formation of blood clots and cause a stroke.
Congenital
Ventricular septal defect (VSD)
A defect in the septum separating the left and right ventricles, causing increased blood flow from the left to right. This causes the left ventricle to enlarge, which will backup blood into the left atrium. VSDs are one of the most common congenital cardiac anomalies diagnosed in children and the second most commonly diagnosed in adults.
Patent ductus arteriosus (PDA)
A persistent remnant of fetal circulation that should have closed off after birth. The ductus arteriosus is required while still in the womb to provide blood circulation through two major arteries, the aorta, and the pulmonary artery. However, when this does not close after birth, it can lead to cardiac abnormalities such as an enlarged left atrium.
Left atrial enlargement complications and symptoms
Several underlying conditions causing left atrial enlargement can lead to complications and poor outcomes. Atrial fibrillation, for example, is associated with an increased mortality as it is associated with the development of blood clots, which can travel to the brain and cause a stroke. Congestive heart failure, often the result of a left ventricular dysfunction, leads to the development of left atrial enlargement. It can cause several cardiovascular complications from irregular heartbeats to indirect fluid and water retention.
Symptoms of left atrial enlargement often depend on the stage of the condition and may include:
- Increased nighttime urination
- Excessive coughing at night
- Abnormal heartbeat and high blood pressure
- Swelling (edema) in the legs or ankles
- Chest pain, difficulty breathing, especially when lying down
- Fatigue or extreme tiredness
- Inability to perform physical exercise with getting very tired
Diagnosis and treatment of left atrial enlargement
The diagnosis of left atrial enlargement is often suspected based on the presentation of symptoms of an underlying cardiogenic condition. Once other tests addressing these other complications are done to help rule out any potentially life-threatening disorders, additional testing looking at the structure of the heart can be done to see if left atrial enlargement is present.
The most commonly done test to diagnose left atrial enlargement is using imaging methods called echocardiograms. It is done by using sound waves to take pictures of the heart structures. The use of other imaging tests, namely CT or MRI scans, can also be used to diagnose left atrial enlargement.
Depending on the underlying condition, treatment will generally follow suit. For example, treating high blood pressure will involve the utilization of blood pressure medication such as beta-blockers and diuretics. Also, maintaining a healthy diet, limiting salt, and being physically active will all be recommended to help manage blood pressure levels.
Treating mitral stenosis and atrial fibrillation will involve the use of rhythm and rate control medication, in addition to anticoagulant medication to reduce the formation of blood clots. Specifically for mitral stenosis, surgical intervention may be required depending on the severity. For severe cases of AFib where medication is found ineffective, the use of electric cardioversion, pulmonary vein ablation, or pacemaker implantation may be required.
Prevention and prognosis of left atrial enlargement
Advertisement
It is always recommended to seek the advice of a trained medical professional, preferably a cardiologist, when attempting to treat and avoid cardiovascular complications. They will be able to give you sound advice pertaining to your own unique situation and provide treatment accordingly. In the meantime, the following tips may be useful for lowering your risk of developing left atrial enlargement and its complications.
- Reduce stress levels as it may lead to heart rate problems
- Disclose to your doctor any family history of heart or cardiovascular conditions
- Avoid using alcohol and tobacco products.
- Maintain an active lifestyle and maintain a healthy weight
- Control blood pressure and cholesterol levels
- Eat heart-healthy foods that are low in salt and cholesterol
With the available treatments and prevention measures outlined in this article, left atrial enlargement prognosis will depend on the severity of the condition and the management of the causative disorder. With proper treatment and adherence to treatment regimens outlined by your doctor, you can be certain all is being done to help keep your heart working as it should.
Related:
- How to prevent right atrial enlargement: Causes, symptoms, diagnosis, and treatment
- Enlarged heart (cardiomegaly): Causes, symptoms, diagnosis and treatment
