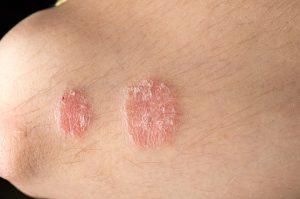
 Psoriasis and psoriatic arthritis increase the risk of gout, as both conditions are associated with the rising levels of uric acid, which breaks down into purines and causes gout. Uric acid builds up in small joints – usually the big toe – where it crystallizes and prompts sudden bouts of intense pain and swelling. If left untreated, gout can become a chronic condition and can contribute to joint damage over time.
Psoriasis and psoriatic arthritis increase the risk of gout, as both conditions are associated with the rising levels of uric acid, which breaks down into purines and causes gout. Uric acid builds up in small joints – usually the big toe – where it crystallizes and prompts sudden bouts of intense pain and swelling. If left untreated, gout can become a chronic condition and can contribute to joint damage over time.
Uric acid can be produced in psoriasis and psoriatic arthritis as a by-product of rapid skin turnover and systemic inflammation.
Advertisement
A 2014 study looked at blood levels of uric acid in 338 psoriasis patients and found that 20 percent of the participants have high levels of uric acid – known as hyperuricemia. The same researchers looked at an alternative 119 psoriasis patients and 119 individuals without psoriasis. They found that psoriasis patients were three times more likely to have high uric acid levels, compared to the controls – even after the results were adjusted for other risk factors.
Additional research published in the Annals of the Rheumatic Diseases looked at nearly 99,000 patients who completed questionnaires about their medical history and lifestyle habits. During the follow-up period, 4.9 percent of men and 1.2 percent of women developed gout. After adjusting for gout risk factors, the researchers found that the risk of gout was double for men and one and a half times greater for women who had psoriasis, compared to those who did not. In patients with psoriasis and psoriatic arthritis, the risk of gout was five times higher, compared to individuals without either condition.
Although there is an extensive body of research that reveals an association between psoriasis, psoriatic arthritis, and gout, there is no cause-and-effect relationship confirmed. The research merely shows an increased risk of gout development and does not necessarily mean that all psoriasis or psoriatic arthritis patients will develop gout.
Psoriasis and psoriatic arthritis treatment options
Treatment for psoriasis depends on the type of disease, the severity, and the body area involved.
For mild disease with only small areas affected, there are topical creams, lotions, and sprays.
For moderate to severe disease affecting much larger areas of the body, topical products may not be effective or practical.
In these cases, doctors often prescribe ultraviolet or other light treatments, or internal medications. Because topical therapy has no effect on psoriatic arthritis, these medications may be necessary to avoid joint deterioration.
Lifestyle measures may bring relief as well, improving the appearance and the feel of damaged skin. Suggestions include:
- Take daily baths: You can relax and de-stress, for one, and bathing will also help to remove scales and calm inflamed skin. Adding in Epsom salts or Dead Sea salts can help with this, too. Tip: Avoid hot water and harsh soaps. Your body needs gentle bathing for effective results.
- Moisturize: Take that extra time to apply a heavy ointment-based moisturizer or oil after bathing, while your skin is still moist. In the colder months, apply moisturizer more than once a day.
- Try sunlight therapy: Exposing your skin to a little sunlight can improve psoriasis. Just don’t go overboard, because too much can worsen outbreaks. On the same note, protect your skin with a sunscreen.
There is currently no cure for psoriatic arthritis, but treatment options are available. Medical treatments involve the use of anti-inflammatory medications, disease-modifying anti-rheumatic drugs (which slow down disease progression), immunosuppressants (medications to lower the function of the immune system), steroid injections (to reduce inflammation quickly), and joint replacement surgery.
Home remedies for psoriatic arthritis include exercising, protecting your joints, maintaining a healthy weight (extra weight adds stress to your already painful joints), and using cold and hot packs to reduce inflammation. Diet, too, can play a role in treating psoriatic arthritis.
Advertisement
Here is a list of foods you should add to your diet to better manage psoriatic arthritis. These foods have been shown to help reduce inflammation.
- Garlic
- Salmon (or fatty fish)
- Cherries and berries
- Whole grains
- Kale (and other dark leafy greens)
On the other hand, there are foods which you should limit or avoid, as they may aggravate psoriatic arthritis and promote inflammation. They are:
- Sugary beverages, like soda
- Nightshade vegetables (tomatoes, eggplants, peppers)
- Fatty red meat
- Dairy
By knowing what to eat and what to avoid, you can ease the symptoms associated with psoriatic arthritis and reduce flare-ups.
