 Ulcerative colitis is a chronic inflammatory bowel disease that impacts about 700,000 Americans. The combination of inflammation and ulcers developed with this disease leads to a lot of discomfort, as well as frequent emptying of the colon.
Ulcerative colitis is a chronic inflammatory bowel disease that impacts about 700,000 Americans. The combination of inflammation and ulcers developed with this disease leads to a lot of discomfort, as well as frequent emptying of the colon.
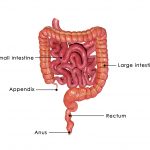
When someone is suffering from this inflammatory bowel disease, the innermost lining of their large intestine (colon) and rectum is affected. The symptoms of ulcerative colitis develop gradually and can be life-changing, making it difficult for some sufferers to maintain normal activities. In many cases, people with ulcerative colitis are fearful of being too far away from a washroom.
Advertisement
Unfortunately, there is no cure for inflammatory bowel disease, but there are ways to reduce the symptoms and bring about periods of remission.
Ulcerative colitis causes and risks
Ulcerative colitis causes are still a source of much research. The exact cause is currently unknown. Medical scientists do believe there are a number of factors that may contribute to increasing a person’s risk of getting the inflammatory bowel disease though.
Some experts point to an overactive intestinal immune system. They believe bacteria or viruses mistakenly trigger the immune system to attack the inner lining of the colon. Others suspect that environmental factors play a big role. Studies have shown that some substances, including antibiotics, oral contraceptives, as well as a high-fat diet may slightly increase the chance of getting ulcerative colitis. There are also those who suggest emotional stress can cause the condition.
Research does indicate that certain abnormal genes could appear in people with the inflammatory bowel disease, suggesting that the condition is genetic. Still, scientists have not been able to make a clear association between genes and ulcerative colitis. What they can tell us is that people are more likely to develop ulcerative colitis symptoms if they are older than 60, if they have a family member with inflammatory bowel disease, or if they are of Jewish descent. Researchers have also discovered that ulcerative colitis is unlikely to occur in people under the age of 15.
Ulcerative colitis signs and symptoms
The most common ulcerative colitis symptoms are abdominal discomfort and diarrhea. However, the signs and symptoms will be different depending on how severe a person’s condition is and where exactly the inflammation takes place in the intestine. Some people can suffer from a mild case of colitis for many years and experience mild symptoms, while others struggle with terrible pain and discomfort.
Here are some typical signs and symptoms of ulcerative colitis:
- Feeling tired
- Nausea or loss of appetite
- Weight loss
- Anemia (fewer red blood cells than normal)
- An urgent need for bowel movement
Some less common symptoms include joint pain, eye irritation, and rashes. Research shows that about 10 percent of people with ulcerative colitis experience severe symptoms, which can include bloody bowel movements and severe abdominal pain.
Ulcerative colitis diagnosis and treatment
 Since some ulcerative colitis symptoms are similar to Crohn’s disease, it is important to get a thorough examination and diagnosis. Ulcerative colitis diagnosis is conducted through a number of tests. Essentially, it is a process of eliminating other conditions. If your doctor suspects an inflammatory bowel issue, he or she may conduct one or more of the following:
Since some ulcerative colitis symptoms are similar to Crohn’s disease, it is important to get a thorough examination and diagnosis. Ulcerative colitis diagnosis is conducted through a number of tests. Essentially, it is a process of eliminating other conditions. If your doctor suspects an inflammatory bowel issue, he or she may conduct one or more of the following:
- Stool tests
- Endoscopy – a flexible tube is used to examine the small intestine
- Colonoscopy – a flexible tube inserted into the rectum to examine the colon
- Biopsy – an examination of tissue removed from the colon, likely during colonoscopy.
- Barium enema – X-rays taken of colon and rectum, using barium to provide contrast.
- Blood tests – to check for low blood count and C-reactive proteins.
If a diagnosis of ulcerative colitis is confirmed, the doctor will discuss the best possible treatment options. Ulcerative colitis treatment can involve drug therapy, surgery, or in cases where the condition is mild, it can simply mean lifestyle changes.
In some instances, medications are prescribed to help reduce inflammation. Reducing the inflammation can minimize both abdominal cramps and diarrhea. Serious inflammatory bowel disease may require antibiotics or other medications to alter immune function.
When symptoms of ulcerative colitis are severe, hospitalization may be necessary. Oftentimes, severe cases lead to dehydration and malnutrition. Severe symptoms could be a sign of a perforated colon or even cancer. Surgery may be required. There are two surgical options: one that involves removal of the entire colon and rectum, called a protocolectomy, and the other involves removal of part of the colon. This is called, ileonal anastomosis. When a protocolectomy is performed, a surgeon makes a small opening in the abdominal wall to bring the tip of the lower small intestine through the skin’s surface. Waste is then drained through the opening into a bag. With the ileonal anastomosis, feces can still pass through the rectum since the rectum is still intact, but the movements will be frequent and watery.
If ulcerative colitis goes undiagnosed and untreated, inflammation can spread, causing problems with other organs and potentially leading to cancer, so proper care and treatment is vital.
Ulcerative colitis prevention and home remedies
While research into eating habits and inflammatory bowel disease continues, patient reports from around the globe indicate that changes in diet and lifestyle seem to help control symptoms and flare-ups for many who have the condition. It appears as if certain foods and beverages aggravate a lot of people who have ulcerative colitis.
Fried foods, sauces, dairy products, spicy dishes, raw vegetables, high-fiber foods, alcohol, and caffeine seem to be problems. An ulcerative colitis diet is one that involves using an enzyme product, such as Lactaid if you want to consume dairy. It also means steaming, baking or stewing vegetables instead of eating them raw, and avoiding butter and margarine, as well as carbonated drinks that produce gas.
If you suffer from ulcerative colitis you may also find that eating several small meals a day, as opposed to three large meals, will make you feel better. Since you aren’t absorbing nutrients as well with ulcerative colitis, you may want to talk to a nutritionist or doctor about taking vitamins.
Advertisement
Some research shows that adding probiotics or good bacteria into our bodies help fight disease. This might be something for people with inflammatory bowel disease to consider. Additionally, studies on herbs and spices are starting to suggest that there could be some therapeutic benefits when fighting ulcerative colitis. Although more research is needed, one of the spices being examined as a possible colitis therapy is curcumin.
Doctors who have treated ulcerative colitis patients say that they have seen great improvements in those who have been able to manage a healthy lifestyle that includes good eating habits, regular exercise, and efforts to eliminate stress.
While it may be true that once you have ulcerative colitis, you have it for life, regular follow-ups with a doctor and careful consideration of how to manage symptoms can make the difference between having a full-life and a reclusive life.
