 Rheumatoid arthritis and gout may appear the same because they cause pain, swelling, and stiffness of joints, but there are very distinct differences between the two. Both conditions can lead to disability and impede on your quality of life, but recognizing the differences can help you choose the appropriate course of action in order to best treat your condition.
Rheumatoid arthritis and gout may appear the same because they cause pain, swelling, and stiffness of joints, but there are very distinct differences between the two. Both conditions can lead to disability and impede on your quality of life, but recognizing the differences can help you choose the appropriate course of action in order to best treat your condition.
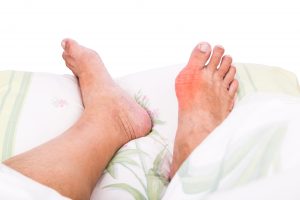
Gout is a condition that affects the small joints in the body – primarily those around the big toe. It is caused by an increase of uric acid, which crystallizes causing redness, pain, and swelling.
Advertisement
Rheumatoid arthritis (RA) is an autoimmune type of arthritis in which the body mistakenly attacks its own joints, once again causing pain, stiffness, and swelling. Here we will explain the other similarities and differences between gout and rheumatoid arthritis in order to increase your understanding of the conditions.
Can you have gout and RA?
Rheumatoid arthritis and gout coexistence is completely possible, mainly because of their differences in causes. Gout is caused by high uric acid levels, primarily due to dietary factors. Therefore, if you have rheumatoid arthritis – an autoimmune disease – and eat a high-uric acid diet, that can cause the formation of gout within rheumatoid arthritis.
Furthermore, the same diet that can contribute to gout can also lead to obesity, adding excess weight onto the joints that are already feeling the pain from RA. This added stress can worsen rheumatoid arthritis symptoms along with gout symptoms. Overall, it’s important to eat a healthy diet and maintain a healthy weight if you are living with gout and RA.
Rheumatoid arthritis vs. gout: U.S. prevalence
 Internationally, rheumatoid arthritis has a prevalence of 0.4 to 1.3 percent. In 2005, it was estimated that 1.5 million U.S. adults had rheumatoid arthritis, and its prevalence is higher among women than men.
Internationally, rheumatoid arthritis has a prevalence of 0.4 to 1.3 percent. In 2005, it was estimated that 1.5 million U.S. adults had rheumatoid arthritis, and its prevalence is higher among women than men.
Prevalence of gout worldwide is one to four percent, and in the U.S. specifically, 3.9 percent of Americans are affected by gout. The authors of the study Global Epidemiology of Gout: Prevalence, Incidences and Risk Factors wrote, “The prevalence of gout in more affluent countries seems to be increasing in recent decades. However, only a few studies give reliable data on secular trends in gout prevalence. The US NHANES study found a significantly higher age-adjusted prevalence (3.9 percent) in 2007–2008 than the estimate in 1988–1994 (2.9 percent). This trend paralleled an observed increase in hyperuricemia.”
Men are at a higher risk of developing gout compared to women, especially those over the age of 40. Individuals who have undergone an organ transplant are at a heightened risk for gout as well.
Signs and symptoms of rheumatoid arthritis and gout
Common signs and symptoms of rheumatoid arthritis include:
- Joint pain, tenderness, swelling, or stiffness experienced for at least six weeks
- Morning stiffness lasting for at least 30 minutes or more
- More than one joint affected by swelling, stiffness, or pain
- Symptoms experienced in small joints, such as in the hands or feet
- Same joints on either side of the body affected
- Dryness and pain in the eyes along with sensitivity to light
- Dryness and gum irritation in the mouth
- Small lumps under the skin
- Shortness of breath and scarring of the lungs
- Inflammation of blood vessels
- Anemia
Common signs and symptoms of gout are:
- Intense joint pain, especially in the large toe
- Lingering discomfort even after the intense pain has subsided
- Inflammation and redness of the affected joint
- Limited range of motion
If a fever develops or the joint feels hot to touch, see your doctor right away. Gout can be successfully managed as long as your doctor is aware of your condition.
Rheumatoid arthritis vs. gout: Causes and risk factors
 Rheumatoid arthritis is an autoimmune disease, meaning, the body’s immune system attacks the joints wrongfully, setting off the symptoms associated with rheumatoid arthritis. Inflammation causes the synovium to thicken, which over time destroys the cartilage, allowing bones to rub together.
Rheumatoid arthritis is an autoimmune disease, meaning, the body’s immune system attacks the joints wrongfully, setting off the symptoms associated with rheumatoid arthritis. Inflammation causes the synovium to thicken, which over time destroys the cartilage, allowing bones to rub together.
Risk factors for rheumatoid arthritis include being a female, being over the age of 40, having a family history of RA, smoking, being exposed to environmental pollutants, and being obese.
Gout is a result of crystallized uric acid, which occurs when a person has high levels of uric acid in their blood. Uric acid results from the breakdown of purines found in some foods like red meat and alcohol.
Normally, uric acid passes through our systems and is released through our urine, but with excessively high levels, the uric acid can build up and crystallize in joints and surrounding tissues, causing discomforting symptoms.
Risk factors for gout include eating a diet high in uric acid-promoting purines, being overweight or obese, having an untreated medical condition like hypertension, taking certain medications, having a family history of gout, being male over the age of 40, and recovering from a recent surgery or trauma.
Rheumatoid arthritis and gout comorbidities
Individuals with rheumatoid arthritis have a higher prevalence of cardiovascular disease, infections, mental health conditions, and malignancies such as leukemia or multiple myeloma.
Gout, on the other hand, has been associated with kidney stones and kidney disease (as those are also caused by uric acid), diabetes, sleep apnea, cardiovascular disease, and cancer. Many of gout comorbidities are due to the fact that they share similar risk factors. For example, in both sleep apnea and gout, obesity is a common risk factor, the same can be said for diabetes.
Rheumatoid arthritis and gout complications
Rheumatoid arthritis increases one’s risk for a number of other conditions, including osteoporosis, rheumatoid nodules, dry eyes and dry mouth, infections, abnormal body composition, carpal tunnel syndrome, heart problems, lung problems, and lymphoma. If rheumatoid arthritis is not well managed the risk of these complications rises dramatically.
Gout complications include reoccurring gout (meaning that the patient will experience frequent flares that can cause erosion and damage to the bones), advanced gout (nodules develop beneath the skin – these are known as tophi and can become tender and painful during gout attacks), and kidney stones, which can cause damage to the kidneys if they reoccur.
Diagnosis and treatment options for gout and rheumatoid arthritis
 Properly diagnosing rheumatoid arthritis involves a slew of tests such as a thorough check of a patient’s medical history and family history, a physical exam, blood tests to look for biomarkers like rheumatoid factors – antibodies commonly seen in rheumatoid arthritis, and imaging tests, like X-ray, ultrasound, and MRI to check for any damage that may have occurred to the joints.
Properly diagnosing rheumatoid arthritis involves a slew of tests such as a thorough check of a patient’s medical history and family history, a physical exam, blood tests to look for biomarkers like rheumatoid factors – antibodies commonly seen in rheumatoid arthritis, and imaging tests, like X-ray, ultrasound, and MRI to check for any damage that may have occurred to the joints.
Diagnostic tests for gout include a joint fluid test in which the fluid from the joint is extracted by a needle and tested for uric acid, blood tests to measure uric acid levels, X-ray imaging to rule out other sources of inflammation, ultrasound, and dual energy CT scan to detect urate crystals.
Treatment for rheumatoid arthritis includes the use of a variety of medications, including nonsteroidal anti-inflammatory drugs (NSAIDs) to relieve pain and reduce inflammation, steroids, disease-modifying antirheumatic drugs, which can help slow down disease progression, and biologic agents that target the immune system as it triggers the inflammation.
Physical therapy and surgery may also be viable treatment options for rheumatoid arthritis in order to increase the range of motion or to replace severely damaged joints.
Advertisement
Gout can also be treated with medications, including NSAIDs and other pain relievers. Some medications can be prescribed to prevent gout complications, including medications to block uric acid and medications to improve uric acid removal.
Lifestyle and home remedies can also be utilized to better manage gout including limiting alcoholic and sugary beverages, reducing your intake of high purine foods (like red meat, organ meat, and seafood), exercising regularly, and maintaining a healthy weight.
If you have rheumatoid arthritis and gout together, you may need to combine treatment options for better treating both conditions. Speak to your doctor about your treatment options for both RA and gout.
