 Psoriatic arthritis and osteoarthritis can both affect small joints and can easily be mistaken for each other, but they are two different conditions that require separate treatments.
Psoriatic arthritis and osteoarthritis can both affect small joints and can easily be mistaken for each other, but they are two different conditions that require separate treatments.
Osteoarthritis is a wearing away of cartilage, usually associated with aging. Psoriatic arthritis is an inflammatory condition in which the joints become inflamed and damaged. There can be inflammation in osteoarthritis, but it is not a major characteristic of the condition, so if a person simply treats their osteoarthritis pain with anti-inflammatories, they may not experience much relief. Both osteoarthritis and psoriatic arthritis can lead to bone spurs, so the two conditions sometimes look the same. Researchers report that osteoarthritis is the most common misdiagnosis for psoriatic arthritis.
Advertisement
People who suffer from osteoarthritis experience the bones of the joint rubbing against each other, which causes friction and pain. In the majority of cases, this rubbing affects the hands, knees, hip, and spine. More people have osteoarthritis than any other form of arthritis.
When you suffer from psoriatic arthritis, you can have inflammation of both the skin and the joints. Psoriasis looks like raised, red patches with white areas of inflamed skin along with scales. The tips of the elbows, the knees, scalp, navel, as well as skin around the genital areas are usually affected. About 10 to 30 percent of those who have psoriasis, will develop psoriatic arthritis.
Psoriatic arthritis and osteoarthritis: Overlapping features
So why can psoriatic arthritis be mistaken for osteoarthritis when it sounds so different? This is due to the fact that osteoarthritis (OA) and psoriatic arthritis (PsA) have overlapping features.
Both OA and PsA often begin after the age of 40 and are commonly linked to excess body weight. They are both associated with joint injury. It is important to understand that even though OA is a “wear and tear” disease, there can be inflammation in the early stages. It is also possible that someone can have OA and PsA at the same time. Another shared characteristic is pain in the spine. While this is more common in OA, it can also happen in PsA sufferers.
Although more research is underway, there is some suggestion that psoriatic arthritis may possibly trigger secondary osteoarthritis. In other words, some inflammation from PsA may be able to cause wear and tear.
Osteoarthritis can start with a small joint swelling that looks like psoriatic arthritis. However, it can later develop into a bony growth known as Heberdens or Bouchards nodes. Often, these growths indicate osteoarthritis in the diagnosis, but they can take several years to form.
Tips for identifying psoriatic arthritis and osteoarthritis
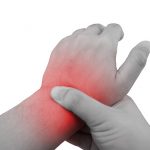 The best way to identify psoriatic arthritis vs. osteoarthritis is to take a close look at unique characteristics or key symptoms. In the case of PsA, increased swelling in the hands and feet can often lead to deformities. Severe foot pain is another common element to watch for. This is due to the arthritis targeting the area in joints where tendons and ligaments attach to the bone. This tends to happen a lot in the Achilles tendons and soles of the feet. People with PsA can also develop a painful swelling in the spinal joints at a point where the spine meets the pelvis. This condition is known as spondylitis.
The best way to identify psoriatic arthritis vs. osteoarthritis is to take a close look at unique characteristics or key symptoms. In the case of PsA, increased swelling in the hands and feet can often lead to deformities. Severe foot pain is another common element to watch for. This is due to the arthritis targeting the area in joints where tendons and ligaments attach to the bone. This tends to happen a lot in the Achilles tendons and soles of the feet. People with PsA can also develop a painful swelling in the spinal joints at a point where the spine meets the pelvis. This condition is known as spondylitis.
Keep in mind that psoriatic arthritis can impact just about any joint. It also attacks in a cycle, with the symptoms growing worse for a period of time and then becoming less severe.
With osteoarthritis, the joints in your body that move the most are more likely to be involved. This includes joints in your hands, knees, feet, and spine. Unlike PsA, it does not cycle. The symptoms grow worse over time and as the disease progresses.
Psoriatic arthritis vs. osteoarthritis: U.S. prevalence
The number of people in the United States who suffer from osteoarthritis is quite astonishing. Research suggests that 70 percent of adults between 55 and 78 years old have OA. Hip osteoarthritis is the most common complaint in North America. Knee is also rather prevalent. Data on osteoarthritis is largely based on self-reports and radiographic data. How does this compare to psoriatic arthritis? The exact number of people in the U.S suffering from PsA is not known, but some estimate it affects around one percent of the population. While it can develop at any time in a person’s life, it seems that most often it occurs between the ages of 30 and 50. While osteoarthritis appears to attack more women than men, psoriatic arthritis attacks men at the same or at a slightly higher rate, compared to women. It is believed that between 18 and 42 percent of people who have psoriasis also have psoriatic arthritis.
Psoriatic arthritis and osteoarthritis: Signs and symptoms
 As we have pointed out, psoriatic arthritis and osteoarthritis share some symptoms, but they also have some differences. Both include joint pain and can produce swelling. However, while psoriatic arthritis is characterized by joint stiffness, osteoarthritis is tender to touch. If you suffer from PsA, you can get psoriasis patches either on or near the affected joint, but if you suffer from OA, you will experience reduced mobility in the affected joint. When a person with OA is mobile, they might feel a grating sensation. The sensation felt by people with PsA is not grating – it is a warm feeling when they touch the joint. Lastly, a person with osteoarthritis may also experience distortions or growths in the joints.
As we have pointed out, psoriatic arthritis and osteoarthritis share some symptoms, but they also have some differences. Both include joint pain and can produce swelling. However, while psoriatic arthritis is characterized by joint stiffness, osteoarthritis is tender to touch. If you suffer from PsA, you can get psoriasis patches either on or near the affected joint, but if you suffer from OA, you will experience reduced mobility in the affected joint. When a person with OA is mobile, they might feel a grating sensation. The sensation felt by people with PsA is not grating – it is a warm feeling when they touch the joint. Lastly, a person with osteoarthritis may also experience distortions or growths in the joints.
The pain experienced by PsA sufferers is often in the fingers, toes, buttock, and spine. The pain for osteoarthritis sufferers is most common in weight-bearing joints, such as the knees, hips, neck, and spine.
Difference between osteoarthritis and psoriatic arthritis causes
There is a difference between osteoarthritis and psoriatic arthritis causes. There are certain factors that will put you at a higher risk of getting OA. You do, though, have control over some of these factors.
Here’s a look at some features that influence the cause of osteoarthritis.
- Weight – people who have excess weight are putting added stress on their weight-bearing joints. As well, the fat tissue produces proteins that can cause harmful inflammation around the joints.
- Age – nothing lasts forever, and as we age our joints simply wear out.
- Joint injuries – if you have experienced a sports injury, you can potentially expose your joints to the kind of stress that leads to OA.
- Repetitive activity – certain jobs or activities that put repeat stress on specific joints can cause joint deterioration.
- Genetics – some people just inherit a tendency to develop OA.
- Deformities – some people are born with defective cartilage or bone deformities that increase their risk of osteoarthritis.
Here’s a look at the factors that can cause psoriatic arthritis:
- Genetics – many people with PsA have a family history of either psoriasis or psoriatic arthritis.
- Physical trauma – this could include a viral or bacterial infection in people with an inherited tendency.
- Stress – anxiety can cause flare-ups or trigger psoriasis.
- Medications – certain medications are known to trigger PsA, including Lithium, antimalarials, high blood pressure medications, and the heart drug Quinidine.
Osteoarthritis vs. psoriatic arthritis complications
 Living with osteoarthritis and psoriatic arthritis can be both physically and mentally challenging. These diseases can also lead to complications. In the case of OA, people do not get better, hence the term degenerative. Degenerative essentially implies progressive, irreversible deterioration. Over time, joint pain and stiffness worsen and may get to the point where completing daily tasks is quite a challenge. It is not unusual for people who suffer from osteoarthritis to have to stop working or cease participating in activities that they normally enjoy. There are also situations where joint pain is so severe that a doctor may recommend joint replacement surgery. Hip and knee replacements are two common operations.
Living with osteoarthritis and psoriatic arthritis can be both physically and mentally challenging. These diseases can also lead to complications. In the case of OA, people do not get better, hence the term degenerative. Degenerative essentially implies progressive, irreversible deterioration. Over time, joint pain and stiffness worsen and may get to the point where completing daily tasks is quite a challenge. It is not unusual for people who suffer from osteoarthritis to have to stop working or cease participating in activities that they normally enjoy. There are also situations where joint pain is so severe that a doctor may recommend joint replacement surgery. Hip and knee replacements are two common operations.
While people with psoriatic arthritis experience periods of relief and remission, they too run the risk of difficulties. For example, a small percentage of those who suffer from PsA develop a condition called arthritis mutilans. This is a very painful and disabling form of PsA. Arthritis mutilans causes extreme damage to the small bones in the hands, leading to permanent deformity.
Differentiating osteoarthritis and psoriatic arthritis diagnosis
When we compare psoriatic arthritis and osteoarthritis diagnosis, we focus more on the process of elimination. With osteoarthritis, a doctor will conduct a physical exam, paying close attention to the joints and checking for tenderness, redness, swelling, and range of motion. Imaging and lab tests are also possible. X-rays can show cartilage loss and bone spurs. In complex cases, an MRI can also produce images of bone and soft tissue. As for the lab tests, analyzing blood and joint fluid can be helpful in confirming the diagnosis. On the other hand, there is really no test for psoriatic arthritis. Doctors usually have to rule out other diseases and take a close look at the symptoms a person is experiencing. It is only in later stages of PsA that an X-ray can pinpoint anything. It may show “pencil in a cup”, which is a situation where the end of the bone gets whittled down to a sharp point. This can support a diagnosis of psoriatic arthritis.
It is possible to have gout along with PsA, so if you have a painful foot joint, especially in the big toe, the doctor may order a test for gout. Fluid from the affected joint is drawn and examined. It is important to note that psoriatic arthritis is often misdiagnosed with gout, because PsA patients can have elevated serum uric acid levels caused by taking low-dose aspirin or by increased skin cell turnover.
Comparing psoriatic arthritis and osteoarthritis treatment
 While there is no cure for psoriatic arthritis, doctors have been able to focus on treating symptoms to help patients control the pain associated with the condition. The kind of treatment depends on how severe a person’s symptoms are and how much damage there is to the joints.
While there is no cure for psoriatic arthritis, doctors have been able to focus on treating symptoms to help patients control the pain associated with the condition. The kind of treatment depends on how severe a person’s symptoms are and how much damage there is to the joints.
Here are three main treatments for PsA:
- Medications – prescriptions and over-the-counter medications to reduce inflammation and pain. Medications to suppress the body’s immune system.
- Steroid injections – inserted directly into the joint to reduce inflammation.
- Surgery – joint replacement in severe cases.
Like psoriatic arthritis, the treatment for osteoarthritis is all about reducing pain so the patient can lead a more comfortable and mobile life.
Advertisement
OA treatments include some of the following:
- Medications – prescription and over-the-counter. More severe cases require stronger medications.
- Lifestyle adjustments – diet and exercise to alleviate pressure on joints.
- Injections – corticosteroids and hyaluronic acid to reduce inflammation and increase mobility.
- Complementary therapies – physical therapy, occupational therapy, canes, braces, and other assistance devices to help with changes in abilities.
- Surgery – badly damaged joints replaced with artificial option to decrease pain and improve mobility.
There are, in fact, over 100 different forms of arthritis, but OA and PsA are two prominent types that have altered the lives of millions of Americans. According to the Centers for Disease Control and Prevention, more than one third of adults who have arthritis have said that it limits their work, leisure activities, and social life. The first step to gaining more control over the pain and mobility issues is learning just exactly what kind of arthritis you have and seeking proper treatment. If you are experiencing painful joint symptoms like those described here, it’s important to compare OA and PsA carefully before assuming one or the other is what ails you.
Sources:
http://www.hopkinsarthritis.org/ask-the-expert/psoriatic-arthritis-and-osteoarthritis/
http://www.everydayhealth.com/psoriatic-arthritis/symptoms/psoriatic-arthritis-and-other-arthritis-forms/
http://www.webmd.com/rheumatoid-arthritis/guide/most-common-arthritis-types
http://enthesis.info/spondyloarthritis/psa_or_osteoarthritis.html
http://www.rheumatologynetwork.com/psoriatic-arthritis/psa-oa-cases-joint-confusion
http://www.healthline.com/health/psoriatic-arthritis-vs-osteoarthritis
http://www.clevelandclinicmeded.com/medicalpubs/diseasemanagement/rheumatology/osteoarthritis/
http://emedicine.medscape.com/article/330487-overview#a6
http://blog.arthritis.org/psoriatic-arthritis/psoriatic-arthritis-psoriasis/
http://www.arthritis.org/about-arthritis/types/osteoarthritis/symptoms.php
http://www.arthritis.org/about-arthritis/types/psoriatic-arthritis/symptoms.php
http://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/dxc-20198250
http://www.mayoclinic.org/diseases-conditions/psoriatic-arthritis/basics/risk-factors/con-20015006
https://www.psoriasis.org/psoriatic-arthritis/diagnosis/tests-to-confirm
