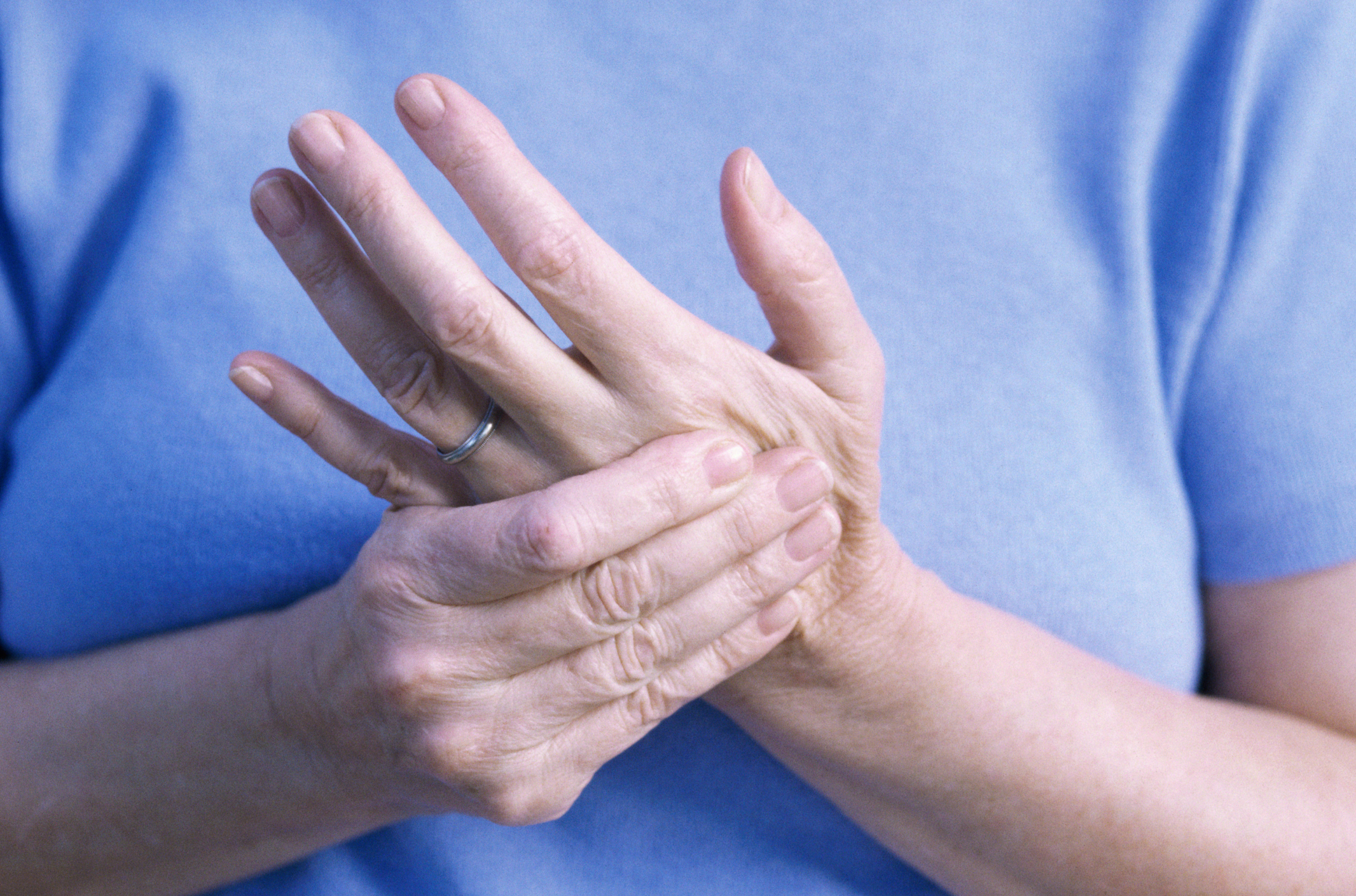
Fibromyalgia and psoriatic arthritis may appear the same, symptomatically speaking, but they are two unique conditions with differences in their symptoms, causes, and treatments. Psoriatic arthritis is a type of inflammatory arthritis that causes inflammation around the joints and tissues. Over time, long-standing inflammation can cause deformation and disability. Psoriatic arthritis is commonly seen in psoriasis patients, but the two conditions are not necessarily comorbid all the time.
and psoriatic arthritis may appear the same, symptomatically speaking, but they are two unique conditions with differences in their symptoms, causes, and treatments. Psoriatic arthritis is a type of inflammatory arthritis that causes inflammation around the joints and tissues. Over time, long-standing inflammation can cause deformation and disability. Psoriatic arthritis is commonly seen in psoriasis patients, but the two conditions are not necessarily comorbid all the time.
Fibromyalgia can affect the joints along with the muscles, tendons, and other soft tissues, resulting in pain experienced all over the body. Fibromyalgia may be a standalone condition or is can coexist with a type of arthritis. Living with both fibromyalgia and arthritis can be quite challenging, but it’s important to tackle both illnesses.
Fibromyalgia and psoriatic arthritis together
Advertisement
Fibromyalgia has been linked to many other health conditions including chronic fatigue syndrome and irritable bowel syndrome. The link may stem from adrenal fatigue and vagus nerve dysfunction. Fibromyalgia and psoriatic arthritis may be linked as well, as outlined in a study looking at 78 individuals of which 34 were diagnosed with psoriatic arthritis.
Of these 38 psoriatic arthritis patients, 53 percent also had fibromyalgia, compared to the 4.3 percent among patients who did not have arthritis.
As mentioned, fibromyalgia and psoriatic arthritis share common symptoms including fatigue, sleep disturbances, limited range of motion, and numbness or tingling.
In order to properly diagnose one or the other, it’s important to determine the underlying cause of pain in order to create a treatment plan.
Fibromyalgia vs. psoriatic arthritis: U.S. prevalence
Fibromyalgia affects roughly two percent of the American population, an estimated five million people. Generally, women have higher rates of fibromyalgia than men, and the condition is commonly diagnosed during middle age.
On the other hand, psoriasis – which is a precursor to psoriatic arthritis – affects as many as 7.5 million Americans. According to the Centers for Disease Control and Prevention (CDC), rates of psoriatic arthritis are about 10 to 20 percent among psoriasis patients, but the International Federation of Psoriasis Associations suggests that rates are higher – 30 to 50 percent.
 Fibromyalgia and psoriatic arthritis signs and symptoms
Fibromyalgia and psoriatic arthritis signs and symptoms
The main symptom of fibromyalgia is widespread pain, but it can more specifically include chronic muscle pain, spasms or tightness, moderate to severe fatigue, low energy, insomnia, waking up tired, stiffness upon awakening or after being in one position for too long, difficulty remembering and concentrating, fibromyalgia brain fog, abdominal pain, bloating, nausea, constipation, tension or migraine headaches, jaw and facial tenderness, sensitivity to light or odors, anxiety or depression, numbness or tingling or limbs, irritable bladder, reduced tolerance for exercise or physical activity, and feeling of swelling in the hands and feet.
Symptoms of psoriatic arthritis are similar to other forms of arthritis and include painful swollen joints, stiffness, swollen fingers or toes (look like sausages), tendon or ligament pain, skin rashes and changes to the finger or toe nails, fatigue, reduced range of motion, inflammation and redness of the eyes, and flares of symptoms, meaning they may strike and last for a while and then go away.
Causes of fibromyalgia and psoriatic arthritis
The cause of fibromyalgia is largely theorized, as it is not well understood. Researchers and doctors believe that a fibromyalgia patient experiences amplified pain as a result of abnormal sensory processing in the central nervous system. Much research has detected physiological abnormalities in fibromyalgia, including increased levels of substance P in the spinal cord, low levels of blood flow to the thalamus region of the brain, HPA axis hypofunction, low levels of serotonin and tryptophan, and abnormalities in cytokine function. Other fibromyalgia triggers include genetic factors and traumatic events or injuries.
Like many other forms of arthritis, psoriatic arthritis is onset when the body’s immune system attacks itself. This means healthy cells are put under attack, which leads to inflammation in the joints and overproduction of skin cells.
Not much is known about why the body would start attacking its own healthy cells, but both environmental and genetic factors may be responsible. Research has uncovered some genetic markers that increase a person’s risk of developing psoriatic arthritis.
Fibromyalgia and psoriatic arthritis: Risk factors and complications
 Risk factors for fibromyalgia include sex – women are at a higher risk of fibromyalgia than men, a family history of fibromyalgia – a genetic component to the disease, and a rheumatic disease diagnosis. Risk factors for psoriatic arthritis include a family history, a diagnosis of psoriasis, and age – psoriatic arthritis is commonly seen in those between 30 and 50.
Risk factors for fibromyalgia include sex – women are at a higher risk of fibromyalgia than men, a family history of fibromyalgia – a genetic component to the disease, and a rheumatic disease diagnosis. Risk factors for psoriatic arthritis include a family history, a diagnosis of psoriasis, and age – psoriatic arthritis is commonly seen in those between 30 and 50.
Fibromyalgia complications include poor ability to function due to lack of sleep, which worsens symptoms. Anxiety and depression, too, may be a result of fibromyalgia as it is not a well understood condition, so it can be frustrating to be living in pain when many others simply don’t understand, especially because there is no specific cure or treatment.
For psoriatic arthritis, a small number of patients will develop arthritis mutilans, which is severely painful and disabling. Arthritis mutilans destroys small bones causing deformities and disability.
Fibromyalgia vs. psoriatic arthritis: Diagnosis
To diagnose psoriatic arthritis, your doctor will closely examine your joints for swelling, stiffness, and tenderness, check your fingernails for flaking and other abnormalities, and press the soles of your feet for any tender points. Although there isn’t a specific test for psoriatic arthritis, other forms of testing can rule out other causes of joint pain and stiffness to narrow down the diagnosis. Other tests your doctor may utilize include X-ray, MRI scans, blood test for rheumatoid antibodies – their presence suggests a diagnosis of rheumatoid arthritis and not psoriatic arthritis, and lastly, a joint fluid test where a doctor inserts a needle to withdraw fluid from the affected joint and check for uric acid to rule out gout.
There isn’t a specific test for fibromyalgia either, but doctors may use a form of testing that checks 18 specific trigger points, which have been found to be in majority of fibromyalgia patients. Not all doctors use trigger point exams anymore, but rather they narrow in on a fibromyalgia diagnosis if a person has experienced widespread pain for at least three months. Your doctor may also refer you for some blood work to rule out other conditions.
Treatment options for fibromyalgia and psoriatic arthritis
 Treating fibromyalgia can be difficult as its exact cause is unknown. Therefore, the goal of fibromyalgia treatment is symptom management. A doctor may prescribe analgesics, or painkillers, to address fibromyalgia. However, there is a risk of developing an addiction to these drugs, so doctors may recommend this option with caution. Nonsteroidal anti-inflammatory drugs (NSAIDs) can also be taken for pain management, but once again long-term use of these drugs can yield unwanted side effects. In some cases, antidepressants may be prescribed as well.
Treating fibromyalgia can be difficult as its exact cause is unknown. Therefore, the goal of fibromyalgia treatment is symptom management. A doctor may prescribe analgesics, or painkillers, to address fibromyalgia. However, there is a risk of developing an addiction to these drugs, so doctors may recommend this option with caution. Nonsteroidal anti-inflammatory drugs (NSAIDs) can also be taken for pain management, but once again long-term use of these drugs can yield unwanted side effects. In some cases, antidepressants may be prescribed as well.
Advertisement
Some alternative and complementary therapies and treatments for fibromyalgia include massages, acupuncture, cognitive behavioral therapy, movement therapies, and chiropractic.
There is currently no cure for psoriatic arthritis, but treatment options are available. Medical treatments involve the use of anti-inflammatory medications, disease-modifying anti-rheumatic drugs (to slow down progression), immunosuppressants (to tame the immune system), steroid injections (to reduce inflammation quickly), and joint replacement surgery.
Home remedies for psoriatic arthritis include exercising, protecting your joints, maintaining a healthy weight – extra weight adds stress to already painful joints, and using cold and hot packs to reduce inflammation. Diet, too, can play a role in treating psoriatic arthritis.
