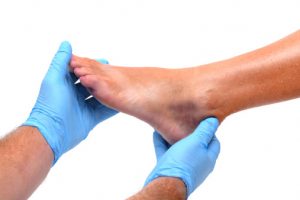
 Diabetes can lead to many complications, such as gangrene and even foot amputation. In diabetes there is an inability to control blood sugar that results in spikes and drops. When blood sugar is not regulated it can lead to nerve damage and impair the body’s ability to fight off infection. For these reasons, foot infections can be a common complication related to diabetes.
Diabetes can lead to many complications, such as gangrene and even foot amputation. In diabetes there is an inability to control blood sugar that results in spikes and drops. When blood sugar is not regulated it can lead to nerve damage and impair the body’s ability to fight off infection. For these reasons, foot infections can be a common complication related to diabetes.
Because the feet are commonly exposed to injury from daily living, the risk of foot infection increases – especially in diabetics. A foot infection for a diabetic may begin as an ulcer but, as the infection becomes deeper, it can lead to gangrene – a condition where the body’s tissues die due to lack of blood and infection.
Advertisement
Nearly half of diabetics will experience a condition of the foot, whether it’s peripheral neuropathy or narrowing of blood vessels, which limits blood flow.
Gangrene, in particular, is the most dreaded foot infection for diabetics. The foot dies and begins decaying, which can ultimately lead to amputation of the foot.
According to the classification system by the National Institute for Health and Care excellence, diabetic foot grading is as follow:
- Grade 0 – when the skin over the foot is intact
- Grade I – superficial or surface ulcer
- Grade II – deeper ulcer
- Grade III – osteomyelitis or bone affliction and/or deep abscess
- Grade IV – forefoot (front of the foot) gangrene
- Grade V – hindfoot (heels and back of the foot affected) gangrene
Diabetic foot complications, gangrene, foot amputation risk
 Researchers used a cross-sectional study of 62,681 patients over the age of 25 to examine foot complications and risk factors. Foot complications among diabetics were 3.3 percent prevalent with a 95 percent confidence interval. Prevalence of foot ulcers, gangrene, and amputations were 2.05, 0.19 and 1.06 percent respectively. With age, foot complication prevalence rose and occurred more often in male participants than female.
Researchers used a cross-sectional study of 62,681 patients over the age of 25 to examine foot complications and risk factors. Foot complications among diabetics were 3.3 percent prevalent with a 95 percent confidence interval. Prevalence of foot ulcers, gangrene, and amputations were 2.05, 0.19 and 1.06 percent respectively. With age, foot complication prevalence rose and occurred more often in male participants than female.
Factors that increased the risk of foot complications in diabetics included Charcot joints, peripheral vascular disease, neuropathy, diabetes duration over 10 years, insulin use, retinopathy, nephropathy, being 45 years and older, cerebral vascular disease (CVD), poor glycemic control, coronary artery disease (CAD), male gender, smoking and hypertension.
For diabetics, not only is it important and vital to control blood sugar to prevent diabetic foot complications, but other listed factors as well should be properly managed.
What is gangrene? Causes and types of gangrene
Gangrene occurs when blood cannot flow to tissues in the body or a bacterial infection is present, both of which cause the tissues to die. This causes decay to that body part. Gangrene can occur in the limbs, organs, and even muscles. Your risk of gangrene increases if you have an underlying condition that limits the supply of blood flow or increases susceptibility to form infection.
Types of gangrene include:
 Dry gangrene: Dry and shriveled skin where the skin changes color. This is most common in blood vessel causes of gangrene.
Dry gangrene: Dry and shriveled skin where the skin changes color. This is most common in blood vessel causes of gangrene.- Wet gangrene: Commonly referred to as wet gangrene if the cause is a bacterial infection. Swelling and blistering may occur and the body part may have a wet appearance.
- Gas gangrene: Commonly affects deep muscle tissues. The surface of the skin may appear normal, but as the condition progresses, skin may turn grey or a purple-red color. Commonly caused by an infection known as Clostridium perfringens, which results from injury or surgery.
- Internal gangrene: Affects internal organs and caused by a blockage of blood flow.
- Fournier’s gangrene: Gangrene of genital organs and typically caused by infection.
- Progressive bacterial synergistic gangrene (Meleney’s gangrene): Rare form that occurs after an operation.
Gangrene and diabetes link
Individuals with diabetes are at an increased risk of developing gangrene. Uncontrolled blood sugar causes damage to nerves and the immune system, which makes it more difficult to fight off infection, thus contributing to gangrene. Roughly one-third of diabetic patients will develop a foot ulcer, which if left untreated or is unable to heal can develop into gangrene.
In gangrene the foot will die and decay, so amputation is the only solution for the foot. It’s estimated that every 30 seconds a foot amputation is conducted worldwide for a diabetic foot ulcer. Furthermore, the death rate due to diabetic gangrene is equal to cancer death rates.
Early signs and symptoms of diabetic gangrene
Signs and symptoms of diabetic gangrene are:
- Discoloration of the skin
- A clear line between healthy and damaged skin
 Severe pain followed by numbness
Severe pain followed by numbness- Foul-smelling discharge from a sore
- Fever
- Low blood pressure
- Rapid heartbeat
- Lightheadedness
- Shortness of breath
- Confusion
Treatment and prevention of gangrene
Tissue that has been affected by gangrene cannot be saved or restored. To stop further progression surgery, medications or hyperbaric oxygen therapy may be utilized.
Surgery involves removing the dead tissue and possibly restoring blood vessels that may be blocked or damaged. A skin graft, too, can be done to repair damaged skin. During a skin graft a doctor will remove healthy skin from another part of the body and reapply it to the affected area. If gangrene is severe a complete amputation will need to be done.
Antibiotics are also utilized to treat gangrene and are administered intravenously. Lastly, hyperbaric oxygen therapy is a procedure where increased pressure and oxygen are used to boost blood flow and help your blood carry greater amounts of oxygen.
Prevention of gangrene is possible; just because you are diabetic does not mean you need to succumb to the condition. Tips to prevent gangrene include:
- Care for your diabetes and ensure blood sugar is well managed.
- Lose weight.
- Don’t smoke.
- Take necessary steps to prevent infection.
- Be mindful of drops in temperature – frostbite can contribute to gangrene as well.
Related Reading:
Stride health: Foot care for diabetics
Diabetics have a lot on their plate. They’re thinking about blood sugar control, following their medication, exercising, watching their carbohydrates and eating right… The list goes on. But feet and diabetes are not always top of mind. We need to change that and put diabetes foot care on the radar. Continue reading…
Advertisement
Neuropathy is the loss of sensation or feeling. It can occur from diabetes (diabetic neuropathy), infection, toxins, drugs, excessive alcohol consumption, inflammatory conditions, it can be hereditary or it can be idiopathic meaning no specific cause is ever found. Continue reading…
Sources:
http://www.mayoclinic.org/diseases-conditions/gangrene/basics/prevention
http://www.ncbi.nlm.nih.gov/pmc/articles
http://www.news-medical.net/health/Diabetes-and-gangrene
http://www.medicalnewstoday.com/articles/158770.php#signs_and_symptoms_of_gangrene
http://www.webmd.com/skin-problems-and-treatments/guide/gangrene-causes-symptoms-treatments
http://www.thehealthsite.com/diseases-conditions/diabetic-gangrene
https://www.nlm.nih.gov/medlineplus/ency/article
