Pulmonary embolism (PE) is probably more common than you might think. More people die from it in the U.S. each year than breast cancer. It happens when a blood clot breaks loose and travels to the heart and lungs.
Legs are the most common place for blood clots, and there are two types.
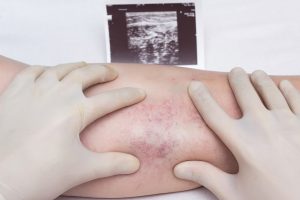
A blood clot in the superficial veins, called superficial venous thrombosis (SVT), can lead to redness, tenderness, or pain. It usually occurs in varicose veins and can lead to more severe clots.
Deep vein thrombosis, or DVT, is more severe. It usually begins in one leg and is marked by swelling and pain. Blood is not able to leave the leg, causing the symptoms. If your leg doesn’t usually swell and it begins to over a couple of days, seek medical assistance. If left untreated, it can lead to PE.
Blood clots happen when blood can’t flow back up through the veins to the heart and lungs to be re-oxygenated. It can pool and clot, leading to potential symptoms. Causes include:
- Being bedridden for an extended period, typically during an illness or following surgery
- Sitting for long periods (even three or four hours)
- Getting too little activity/sitting too much
- Untreated varicose veins/superficial veins that don’t work properly
- Certain medications
- Family history
- COVID-19
- Smoking
- Age
- Obesity
- Heart trouble
Thankfully, you can reduce your risk for DVT in many ways. First, you can assess your risk with various smartphone apps or by talking to your doctor.
But regardless of risk, you want to be proactive in your approach. Here’s what to do:
- Stay hydrated. Drinking plenty of water helps keep blood thin and moving easily through your venous system.
- Stretch your legs every hour or two. Also, make a point of stretching your calves and moving ankles back and forth.
- Move legs while lying down. Bend your knees and pint and flex feet if lying down for an extended period.
- Try compression stockings
- Pay attention to your positioning. Avoid crossing your legs and remember to periodically change your position while seated
- Take breaks during travel. Get up every hour or two to move if on a plane or train, or pull the car over for a brief walk or stretch when driving.