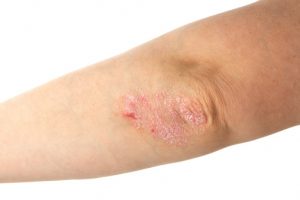
 Psoriasis risk increases with high blood pressure and anti-hypertension drugs. Psoriasis is an immune-related disease affecting nearly three percent of the American population. The researchers found that in women, specifically, long-term hypertension along with the use of anti-hypertension drugs (especially beta-blockers) was associated with a higher risk of psoriasis.
Psoriasis risk increases with high blood pressure and anti-hypertension drugs. Psoriasis is an immune-related disease affecting nearly three percent of the American population. The researchers found that in women, specifically, long-term hypertension along with the use of anti-hypertension drugs (especially beta-blockers) was associated with a higher risk of psoriasis.
The researchers analyzed psoriasis cases in 77,728 women participants in the Nurses’ Health Study from 1996 to 2008. There were 843 incidences of psoriasis.
Advertisement
Women who had had high blood pressure for at least six years were at the highest risk for psoriasis, compared to women with normal blood pressure. The risk was also higher among hypertensive women who did use the medication and who did not use the medication, compared to normal blood pressure women. Those women who regularly used beta-blockers for at least six years were at a high risk for psoriasis as well.
The researchers noted, “These findings provide novel insights into the association among hypertension, antihypertensive medications, and psoriasis. However, further work is necessary to confirm our findings and clarify the biological mechanisms that underlie these associations.”
Psoriasis, hypertension may be strongly linked
In an alternative study, researchers found that patients with psoriasis were at a higher risk for uncontrolled hypertension. The researchers collected data that revealed a strong link between psoriasis and hypertension.
Co-first author Dr. Junko Takeshita said, “Over the last several years, studies have shown that psoriasis, specifically severe psoriasis, is an independent risk factor for a variety of comorbidities, putting patients suffering with this common skin disease at an increased risk for other conditions such as heart attack and stroke. Knowing that psoriasis is tied to other health conditions, it’s vital that we have a better understanding of the systemic effects it has on other areas of the body so that we can more closely monitor these patients and provide better and preventative care.”
The researchers found that severity of uncontrolled hypertension increased with greater severity of psoriasis. Patients at highest risk for uncontrolled hypertension were those who had at least three percent of their body surface covered with psoriasis.
Advertisement
The researchers looked at the patient data from The Health Improvement Network (THIN) and focused primarily on a specific group called the Incident Health Outcomes and Psoriasis Events (iHOPE) cohort.
Dr. Takeshita explained, “Most large electronic databases such as THIN do not have information such as body surface area involvement or other direct measures of psoriasis severity, and we usually have to use surrogate measures such as receipt of a treatment that is indicated for more severe psoriasis to define psoriasis severity. The use of surrogate measures to define psoriasis severity is not ideal for multiple reasons. For example, we know that many patients with psoriasis go untreated, so using treatment to define psoriasis severity may incorrectly identify patients who truly have severe disease as having mild disease. Furthermore, when we use treatments to define psoriasis severity, we cannot separate effects of psoriasis itself from potential psoriasis treatment effects on blood pressure control. To our knowledge, ours is the first study to evaluate the effect of objectively determined psoriasis severity on blood pressure control.”
“Determining the cause and effect is something that needs to be evaluated in future longitudinal studies so that we can better assess which condition developed first. Our hypothesis is that the psoriasis and the inflammation that comes with it are making the hypertension worse, but certainly it could go the other way, and understanding which comes first has important implications for how we care for these patients and our understanding of how these two conditions are related,” Dr. Takeshita concluded.
